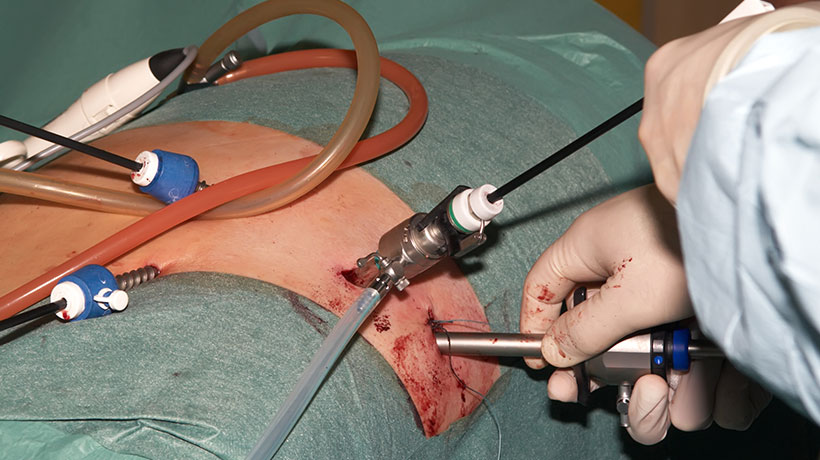
Can weight loss surgery be a cure for diabetes?
Gastric bypass surgery can lead to remission of type 2 diabetes. A recent study published in the American Journal of Physiology — Regulatory, Integrative and Comparative Physiology, aimed to find out why Roux-en-Y bypass surgery improves insulin sensitivity. Insulin transfers sugar from the blood into storage sites around the body, such as skeletal muscle and fat tissue. Poor insulin sensitivity means that that this process is slowed down, leading to a high blood sugar level, this is commonly known as type 2 diabetes and is prevalent in obese people.
The study looked at abdominal fat and thigh muscle samples taken before and after gastric bypass surgery. Significant improvement was seen in insulin sensitivity by 12 months after surgery, with the greatest improvement being noticed in fat tissue, suggesting that it plays a more prominent role in insulin sensitivity than previously thought. Overall, the study suggests interesting interactions between insulin and fat tissue, whilst showing that Roux-en-Y gastric bypass could contribute more in treating insulin sensitivity.
Read More
Bariatric surgery alters our brains
A finnish study has shown that bariatric surgery along with weight loss normalises the brains opioid neurotransmission, which is involved in generating a feeling of pleasure. The research highlights how obesity has an effect at the molecular level within the brain and how much weight loss can affect this. The findings suggest that a lack of opioid receptors (which cause a feeling of pleasure), in the brains of obese individuals, means that they must eat more in order to feel pleasure.
Furthermore, as the levels of receptors normalised after weight loss, it is understood that lower levels in obese people is a consequence of obesity, rather than a cause. This finding helps us understand the molecular involvement of obesity on a much different level than previously thought, and may provide a new option for behavioural and pharmacological treatment.
Read More
How much sugar is too much sugar?
A new study published in the journal Obesity has shown that proposed changes in the ‘Nutrition Facts’ label on food will help people understand how much sugar they are consuming. The Canadian study aimed to test the efficacy of formats for labelling on food, showing the total and added sugar. The researchers conducted studies on 2,000 16-24 year olds and found that adding a percentage daily value for added sugar helped them identify foods with ‘too much’ sugar in.
At first these young people found it difficult to correctly identify foods high in sugar, but with added labels and percentage values they understood more and felt that they would be less inclined to consume those foods high in sugar. The study highlights the fact that whilst it is important to research the different types of treatment for obesity, we must not forget that prevention is better than a cure and that obesity can be stopped by even the simplest of measures.
Read More
Mothers find it difficult to admit that their children are obese
Admitting that they themselves are obese is easier for a mother than admitting their child is. This comes after a study conducted in Ireland found that mothers were more honest and accurate about their own height and weight, but only 17% of mothers of obese children could admit that their child was overweight. This means that they are less likely to seek help and intervene due to their child’s weight, increasing the chances of the child gaining more weight, and eventually tracking this into adulthood.
The effect is more apparent in the cases of overweight daughters, where mothers are far less likely to admit that their daughters were obese than their sons. Identifying the problem is the first step to solving it, and by not recognising their children’s problems some mothers may be subconsciously putting their children at increased health risks. The researchers suggested that the problem may arise due to the fact that mothers are not objectively measuring their children, but could be comparing them to their peers. Furthermore, if a mother does identify her child as overweight, she may feel that she needs to intervene and upset the child, and therefore avoids this. In summary, the study called for more open and honest discussions between health professionals, parents and children in order to maintain healthy weight in the young.
Read More
Obesity rates to soar if no action is taken
New figures suggest that 2.7 billion adults will be obese by 2025. In a press release the World Obesity Federation has estimated that the global prevalence of obesity will be as high as this if current trend continue. The figures were released on the first World Obesity Day on the 11/10/2015. In the release it explains that in 2012 governments around the world committed to bringing levels of obesity back down to those that existed in 2010, by 2025. This was part of an idea developed by the WHO called the Global Action Plan for the Prevention and Control of Noncommunicable Diseases. The report suggests that the governments in question have not been doing enough to control the rise in obesity rates.
The president for the World Obesity Federation, Professor Walmir Coutinho, urged these governments to act immediately in order to halt the rise in the obesity epidemic using measures such as market controls, taxes and subsidies, whilst also setting standards for catering services and investment in healthy schools. Whilst the current prevalence of obesity is 13% worldwide, with this estimated increase it will become 17% by 2025, evidently more action needs to be taken to stop this.
Read More