Sugar substitute may not promote weight loss
A team of researchers from Massachusetts General Hospital have found a possible mechanism that may help explain why aspartame, a sugar substitute, does not help promote weight loss. Their report was published in Applied Physiology, Nutrition and Metabolism, and it explains that phenylalanine, a breakdown product of aspartame may interfere with the actions of an enzyme which prevents metabolic syndrome. Using mouse models, the researchers found that a diet with aspartame actually increases weight, whilst a non-aspartame diet does not.
During this study, a series of experiments was carried out, with one showing that the activity of an enzyme, known as IAP, was greatly reduced when added to a solution containing an aspartame sweetened drink, this was not the case in the sugar sweetened drink. This is particularly worrying as sugar substitutes are often used to promote weight loss by limiting the consumption of sugar. Now a number of epidemiological studies are looking into whether these substitutes are genuinely effective. The researchers want to highlight that other mechanisms may be involved, and this is only one such mechanism that may point to the use of artificial sweeteners being counter-productive.
Read More
Large BMI increase during puberty may predispose to death by cardiovascular disease later in life
A study published in The Lancet Diabetes & Endocrinology has found that boys with a large increase in BMI during puberty are at an increased risk of death due to CVD in later life. The study itself included over 37,000 men born between 1945 and 1961, and the change in BMI was calculated using BMI values at 8 and 20 years of age. The aim of the study was to evaluate the contribution of BMI for cardiovascular mortality, with the focus being the developmental period of puberty.
There was no increase in cardiovascular risk for those who were overweight before puberty, or those whose BMI normalised during puberty. BMI normally increases during puberty, however this study found that when BMI increases by more than 7 units, the risk of cardiovascular mortality later in life is also increased; this is by 22 per cent for every extra BMI unit. The researchers are now urging schools to monitor their students’ BMIs to ensure that they do not suffer from cardiovascular complications in the future.
Read More
Does fatty food cause mental health issues?
A recent study published in Molecular Psychiatry has found that excess fatty intake can affect the cognitive function of brains. This study was conducted in mice, and found that diets rich in fat reduce levels of an important protein called reelin that helps synapses in the brain signal to one another, resulting in possible cognitive and psychiatric issues. Reelin deficiency is also a feature of brain disorders such as schizophrenia and Alzheimer’s disease. The researchers saw changes as early as four weeks into the experiments, after the mice had been fed high-fat diets. The cognitive results were evident even before the animals started gaining weight. Interestingly, the results were only seen in mice that were adolescent and not fully adult mice.
The changes were mostly evident in the prefontal cortex of the mice, in humans, this is associated with decision making, expressing personality and controlling social behaviour. With the supposed drop in the quality of diets over the past few decades, this study has found some worrying results. Furthermore, the study found the results to be particularly pronounced in adolescent mice, in humans this is a period where people will start to make their own decisions about food, especially with increased calorific needs, the researchers have suggested that more education must therefore be provided about the potential pitfalls in choosing high fat diets.
Read More
Diet and exercise improves kidney function in fatty liver patients
Non-alcoholic steatohepatitis (NASH) is characterised by excess fat in the liver that can cause inflammation and scarring. This may progress to cirrhosis and liver cancer; it can also compromise kidney function. A recent study has found that patients with confirmed NASH, who were put on a low-calorie/fat diet and participated in an exercise programme, experienced reduced liver inflammation and an improved kidney function.
These results were seen after controlling for compounding factors such as diabetes, hypertension and medications. However, the exact mechanism by which these outcomes were made is not fully understood yet. The researchers have hypothesised that oxidative stress, insulin sensitivity,inflammation, and vascular endothelial function all have roles to play. Hopefully, more research will be done in this area to fully understand the therapeutic benefits of such programs for patients with NASH.
Read More
Not eating breakfast or getting enough sleep can make children overweight
Mothers smoking in pregnancy, children skipping breakfast, and children not getting enough sleep, all appear to be important factors in predicting whether a child will become overweight or obese. Researchers from UCL have published a paper in Pediatrics that calls for prompt intervention in order to slow the growth of overweight and obesity in children. The paper looked at data from 19,244 families over a 9 year period, using the Millennium Cohort Study. The researchers were using observational information, meaning that they cannot draw firm conclusions, however the sample size was large and they were able to take into account a range of lifestyle factors that could impact the results.
It is already known that children of obese parents are more likely to be overweight themselves; this could be due to their obesogenic environment, or a genetic predisposition. However, this research also highlights the importance of lifestyle choices that can greatly contribute to the risk of obesity. Disrupted routines, as well as a lack of sleep, can increase appetite and the consumption of energy dense foods. Overall, the researchers were hoping to increase parental education with their findings, so that the growth of overweight and obesity can be curbed.
Read More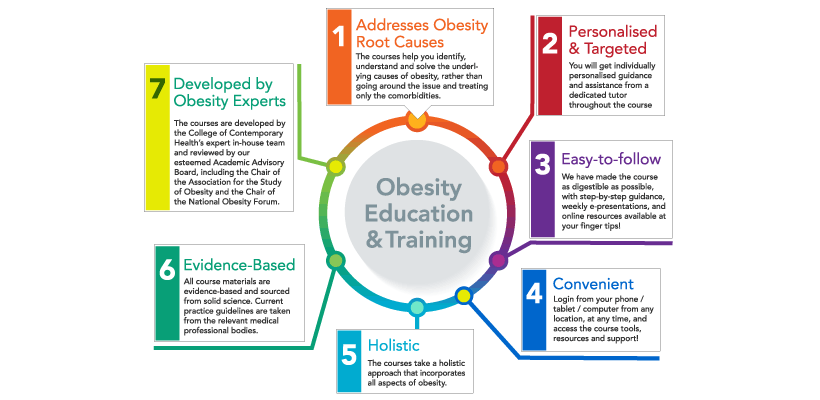
7 reasons to consider an Obesity Care and Weight Management course
We have spoken quite a bit about the need for Obesity Education and Training.
Today, I would like to share with you the top 7 reasons some of our students chose to study Obesity Care and Management with CCH online.
Read More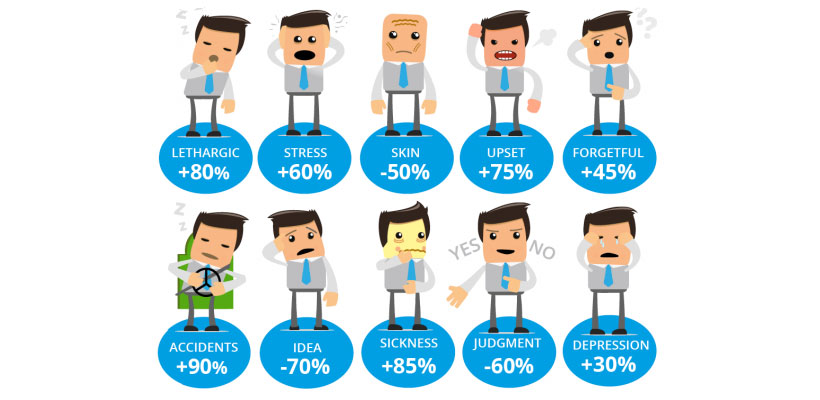
The effects of lack of sleep!
Did you know that an important consideration when treating a patient with overweight and obesity is, sleep apnoea?
Obesity is a major risk factor for the increased incidence of sleep apnoea. Sleep apnoea is a sleep disorder characterised by pauses in breathing or periods of shallow breathing during sleep.
As a person gains weight, especially in the trunk and neck area, the risk of sleep-disordered breathing increases due to compromised respiratory function. As it disrupts normal sleep, those affected are often sleepy or tired during the day.
Read More