
UK and Ireland collaborate for innovation in Digital Health
Ireland and the United Kingdom recently announced a new collaboration aimed at promoting digital innovation in the healthcare sector. The partnership aims to bring together the expertise and resources of both countries in order to create new, cutting-edge solutions for the delivery of healthcare services.
One of the key goals of this collaboration is to develop new digital technologies that can help improve patient outcomes and experiences. This will be achieved through the creation of innovative digital tools and platforms that can help healthcare providers to better manage patient care, as well as through the development of new approaches to medical research and development.
Another important aspect of this collaboration is the sharing of best practices and knowledge between healthcare providers in both Ireland and the UK. This will help to ensure that healthcare providers in both countries are able to stay up-to-date with the latest developments and advancements in digital health.
The collaboration will also focus on the creation of new business opportunities in the digital health sector. This will include the development of new products and services that can help to improve the delivery of healthcare, as well as the creation of new start-ups and spin-off companies that can bring innovative solutions to the market.
Overall, the collaboration between Ireland and the UK is expected to have a positive impact on the healthcare sector, both in terms of patient outcomes and in terms of the growth of the digital health industry. By working together, the two countries hope to establish themselves as leading players in the digital health space and to drive forward innovation and progress in the field.
The partnership is a significant step forward in the ongoing effort to modernise the healthcare sector and to make healthcare services more accessible, efficient, and effective for patients. With the collaboration between Ireland and the UK, we can expect to see a range of new digital health solutions emerging in the coming years, which will help to improve the lives of patients and healthcare providers alike.
Read More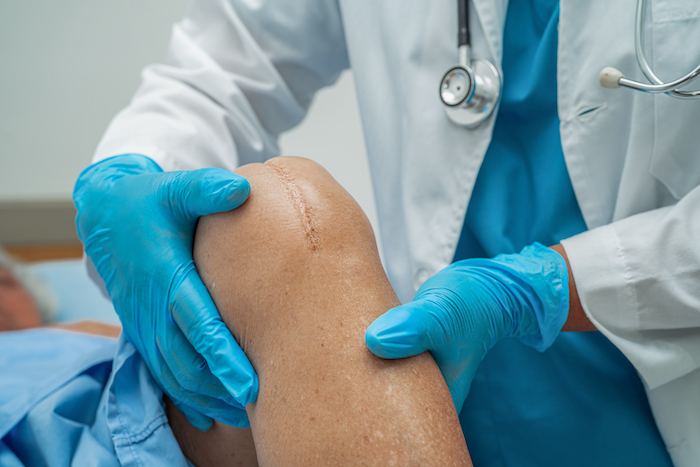
Telehealth programs improve outcomes in patients with knee osteoarthritis, obesity
Telehealth programs have shown to positively impact patients with knee osteoarthritis and obesity. A recent study found that these programs improve patient outcomes by providing convenient access to care, increasing patient engagement and promoting lifestyle changes. The study participants using telehealth reported higher levels of physical activity and better overall knee function compared to those who did not use telehealth. The findings highlight the potential for telehealth to improve the management of chronic conditions and the delivery of care for patients. The results also demonstrate the importance of technology in healthcare, as telehealth programs can bridge gaps in access to care and support better patient outcomes.
Read More
AI chatbots could help patients discuss sensitive health conditions
Artificial Intelligence (AI) technology, specifically chatbots, have the potential to help patients with sensitive health conditions, according to a recent article from Digital Health. Chatbots can provide quick and easily accessible information, support, and guidance to patients, especially those with sensitive health conditions that require constant monitoring and care.
One of the key benefits of chatbots in healthcare is their ability to provide quick and accurate information to patients. Chatbots can answer patients’ questions, provide them with educational materials, and even schedule appointments, freeing up time for healthcare professionals to focus on more complex tasks.
For patients with sensitive health conditions, chatbots can provide emotional support and help manage symptoms. Chatbots can engage in conversations with patients, listen to their concerns, and provide them with coping strategies and resources. This can improve the patient’s overall well-being and help them feel more in control of their health journey.
Chatbots can also assist in monitoring patients’ health status and provide real-time feedback. For example, chatbots can remind patients to take their medications, track their symptoms, and even provide alerts to healthcare professionals if there are any concerning changes in the patient’s condition.
From providing quick and accurate information, to offering emotional support and monitoring health status, chatbots have the potential to play a significant role in the care of patients with sensitive health conditions and can improve the overall experience for patients enhancing the quality of care they receive.
Read More
Minister praises Saudi Arabia’s use of digital health in virus fight
The adoption of digital health technologies as new standards in Saudi Arabia reflects the country’s leadership in international and regional forums, according to Saudi Health Minister and Chairman of the Saudi Health Council, Fahad Al-Jalajel. In his speech at the opening of the HIMSS21 Middle East Health Conference, Al-Jalajel emphasised the crucial role digital technologies played in dealing with the COVID-19 pandemic. The first interactive map of COVID-19 data was launched to provide accurate statistics and employ artificial intelligence to analyse the data and make national strategic decisions.
The HIMSS21 conference aims to discuss current challenges and exchange ideas and experiences in the field of healthcare, both regionally and internationally. The conference will also highlight the importance of health information technology and its role in improving the efficiency of performance, enhancing the quality of services, and optimising the use of resources.
Innovative plans are being implemented in Saudi Arabia to develop the health system, including building a health transformation plan and designing programs for governing, financing, and providing health services. Digital health is a critical partner in this transformation, in line with the National Transformation Program and the country’s Vision 2030.
Secretary-General of the Saudi Health Council, Dr. Nahar Al-Azmi, stated that the HIMSS21 conference will also address the current challenges in the health sector and propose visions and ideas for future plans and potential solutions. The conference will provide an opportunity for exchanging knowledge, experiences, and expertise, as well as global dialogues on the challenges facing health systems and the available solutions. The goal is to harness digital health to build effective responses to future epidemics, benefit from data and technology to enhance population health management, and adopt digital health technologies as new standards to improve the quality of healthcare.
Read More
Scant obesity training in medical school leaves doctors ill-prepared to help patients
Published in NPR, “Scant Obesity Training in Medical School Leaves Doctors Ill-Prepared to Help Patients” highlights the lack of obesity education in medical schools, leaving doctors unprepared to help patients with obesity. According to the article, only about 25% of U.S. medical schools require a course on nutrition and only about half require a course on obesity. The article argues that this lack of training leads to missed opportunities for doctors to help patients manage their weight and can result in patients not receiving the care they need. It also notes that the COVID-19 pandemic has only magnified the need for medical professionals to be equipped to address obesity, as people with obesity are at higher risk for severe illness from the virus.
Read MoreHigher obesity levels linked to lower productivity in England, research shows
Published in The Guardian, “Higher obesity levels linked to lower productivity in England, research shows” discusses the findings of a new study that shows a correlation between obesity levels and lower productivity in England. The study found that people with obesity tend to miss more work days due to health issues and are less productive when they are at work, leading to a loss of economic output for the country. The article notes that the findings of the study have implications for both employers and policymakers, as addressing obesity and promoting healthy lifestyles could lead to improved health and increased productivity for the workforce. The article also highlights the need for comprehensive programs and policies aimed at reducing obesity levels and improving overall health in England.
Read More
Only eating between 7am and 3pm helps people with obesity lose weight
Published in New Scientist, “Only eating between 7am and 3pm helps people with obesity lose weight” describes the results of a study that found that time-restricted eating (TRE) can be an effective tool for weight loss in people with obesity. The study found that individuals who only ate between the hours of 7am and 3pm lost an average of 8% of their body weight in just 12 weeks. The article notes that the benefits of TRE go beyond weight loss, as it has also been linked to improved metabolic health, reduced inflammation, and better sleep. The article suggests that TRE could be a simple and effective way for people with obesity to improve their health, but more research is needed to fully understand the effects of this eating pattern.
Read More
France sees a surprising surge in obesity
An article in The Economist titled “France sees a surprising surge in obesity” highlights the recent increase in obesity rates in France. The article notes that despite being known for its healthy eating habits and cuisine, France is experiencing a rise in obesity levels, particularly among children, and attributes the increase to a shift towards more sedentary lifestyles, as well as the availability of unhealthy food options. The article also discusses the potential health consequences of the trend and the need for public health initiatives to address the issue. The article concludes by stating that the obesity epidemic is a growing concern in many countries, and addressing the issue will require a multi-faceted approach, including changes in government policies, increased access to healthy food, and increased physical activity.
Read More
Taxing sugary drinks may not cut obesity as much as headlines claim
An article published in New Scientist titled “Taxing sugary drinks may not cut obesity as much as headlines claim” examines the impact of taxing sugary drinks on obesity rates. The article cites studies that have shown that taxing sugary drinks has had limited success in reducing obesity rates, as consumers often turn to other sources of added sugar, such as snacks and desserts. The article notes that while taxing sugary drinks may be a step in the right direction, it is not a silver bullet solution to the obesity epidemic, suggesting instead that a comprehensive approach to reducing obesity is needed, including changes in government policies, increased access to healthy food, and increased physical activity. It concludes by stating that while taxing sugary drinks may have some impact on reducing obesity, it is not a complete solution, and additional efforts are needed to address the issue.
Read More
Meet Mel Idroos, CCH PGDip Graduate!
Meet Mel Idroos, PGDip in Lifestyle Medicine (Obesity Care) graduate!
Having completed one of our CPD Short Courses in 2015, Mel decided to expand upon her new knowledge base by taking the plunge and beginning her postgraduate studies with the College of Contemporary Health (CCH).
Beginning in September of 2020, with the ambitions of deepening her knowledge of obesity and enhancing her clinical practice, Mel graduated from CCH in September of 2022 with a Postgraduate Diploma (PGDip) in Lifestyle Medicine (Obesity Care) with Merit.
Since her graduation, Mel has already begun to put what she’s learned into practice developing and delivering Tier 2 adult weight management services, making a meaningful impact in the lives of her patients with obesity.
Here we have interviewed Mel about the impact she is making with her Postgraduate Diploma from CCH:
Q: Hi, Mel! Where do you work at the moment?
A: I work for a Community Interest Company. We are contracted by the local county council to deliver a Tier 2 adult weight management service.
Q: What profession do you work in?
A: I work in the Well-being directorate. As well as adult weight management we deliver a range of health and well-being services to the local population.
Q: Who are some of the patients you assist on a day-to-day basis?
A: We see a wide range of clients in our weight management service. Almost all have a long-term condition associated with excess weight and have tried multiple approaches to lose weight over many years.
Q: What percentage of your patients have overweight or obesity?
A: All clients who come to the service, either as a self-referral or through an HCP referral, have overweight or obesity. The average referral BMI is 36.
Q: What inspired you to study Lifestyle Medicine (obesity care)?
A: I wanted to deepen my knowledge of obesity and enhance my clinical practice as well as cascading what I have learnt to our team of practitioners.
Q: Why did you choose CCH?
A: Working full-time I was attracted to the flexibility of CCH’s online learning. I particularly enjoyed the variety of module options offered. Paediatric Obesity’ and ‘Obesity and Reproductive Health’ were 2 modules that offered entirely new areas of study for me

Q: How did gaining your PGDip at CCH enhance the care that you provide to your patients?
A: I used the information gained through studying the PGDip to enhance and augment our core programme ‘My Weight Matters’. I was able to write new content for the course covering topics not previously included. Sleep, stress, mindful eating practices and social support are just some of the information I was able to add. The course’s behaviour change and psychological aspects were valuable in enhancing the quality of our 1-1 and group interventions.
Q: What has changed most in your practice since starting your studies?
A: The course has given me more confidence to answer those tricky and complex questions that clients often ask!
Q: What is one of the biggest takeaways you gained from your PGDip as a health professional?
A: The topic of weight stigma really struck a chord with me. I have an idea for a piece of work in this area and hope to implement this across our service very soon.
Q: Would you encourage other health professionals to pursue a PGDip with CCH?
A: I would absolutely encourage other health professionals to pursue this course. Much of what I have learnt I have already put into practice.
Q: What is the main reason you would recommend CCH courses to your colleagues?
A: I would recommend this course due to the high-quality materials offered to engage with, and the diversity of topics covered. The tutor support is excellent. The online, flexible approach was also highly-valuable to me.
The College of Contemporary Health, with the University of Central Lancashire Medical School, offers the first, and only, fully online postgraduate qualifications (PGCert/PGDip/MSc) in Lifestyle Medicine (Obesity Care) not just for UK based students, but for students across the world.
We offer 3 student intakes per year starting in January, May, and September.
Click here to apply: Apply for a Postgraduate Qualification in Lifestyle Medicine (Obesity Care).
Read More
Positive parenting can reduce the risk that children develop obesity
Children with positive, early interactions with their caregivers — characterised by warmth, responsiveness, and a stimulating home environment — were at reduced risk of childhood obesity according to new research from Pennsylvania State University in the United States.
The study, “Family Psychosocial Assets, Child Behavioral Regulation, and Obesity,” appeared in the journal Pediatrics. In the article, Brandi Rollins, assistant research professor of biobehavioural health and Lori Francis, associate professor of biobehavioural health, analysed data from over 1,000 mother-child pairs and found that children’s early exposures to family psychosocial assets — including a quality home environment, emotional warmth from the mother, and a child’s ability to self-regulate — reduced the risk of developing childhood obesity.
“A lot of the discussion around childhood obesity and other health risks focuses on identifying and studying the exposure to risk,” said Rollins, “We took a strength-based approach in our analysis. We found that a supportive family and environment early in a child’s life may outweigh some of the cumulative risk factors that children can face.”
An especially encouraging aspect of the study found that these factors were protective even when children faced familial risks for obesity, including poverty, maternal depression, or residence in a single-parent home.
“Research on parenting has shown that these types of family assets influence children’s behaviour, academic success, career, and — not surprisingly — health,” Rollins said. “It is significant that these factors also protect against childhood obesity because the family assets we studied are not food or diet-specific at all. It is heartening to know that, by providing a loving, safe environment, we can reduce the risk that children will develop obesity.”
Children are deemed to have obesity when their body mass indices (BMIs) are greater than 95% of other children their age and gender. There is a great deal of variance, however, in the BMIs of children who exceed the obesity threshold. Children whose BMI is 20% higher than the obesity threshold are considered to have severe obesity.
The researchers found that children who had early-onset severe obesity did not face greater levels of family risk than children who were not obese. Children with severe obesity, however, did have fewer family assets than children who were not obese or who displayed moderate levels of obesity. More research is needed to understand which factors contribute to the development of severe obesity and which factors reduce the risk.
“Though the findings on severe obesity may seem discouraging, they offer some hope,” Rollins explained. “Some risk factors, like household poverty, can be very difficult to change. Assets, on the other hand, may be easier to build. People can learn to parent responsively. It is encouraging that parenting really matters, that family matters.”
Read More
Europe set to miss global heart health targets as obesity skyrockets
According to a paper published in European Heart Journal, the flagship journal of the European Society of Cardiology, the prevalence of obesity in Europe has more than doubled over the past 35 years, with over one in five adults affected.
The third report from the ESC Atlas Project updates and expands upon the previous edition with cardiovascular disease (CVD) statistics to 2019, or the latest available year, for the 57 ESC member countries.
CVD is the most common cause of death in the region, accounting for 45% and 39% of fatalities in women and men, respectively. Unfortunately, the report paints a picture of ageing populations and low birth rates. Between 1970 and 2019 the proportion of individuals aged over 65 years increased from a median 9.2% to 17.2%, and the median age increased from 29.6 to 41.1 years. Alongside this, between 1970 and 2018 fertility rates fell from 2.6 to 1.6, below the average of 2.1 live births per woman needed for population replacement.
Each year, an estimated 48,000 new cases of coronary heart disease occur across Europe due to environmental noise pollution.
Professor Adam Timmis, chair of the report writing team, said, “Sociodemographic and environmental risk factors receive relatively little attention from cardiologists but make a substantial contribution to the risk of CVD. Europe now has top-heavy populations and this will exacerbate the growing burden of CVD. The situation is compounded by increasing urbanisation which threatens heart health due to dirty air, noise, social deprivation and stress. It is estimated that up to 40% of people living in the EU are exposed to noise levels beyond the region’s residential limits.”
According to the World Health Organisation (WHO), noncommunicable diseases kill 41 million people each year, equivalent to 71% of all deaths globally. CVD accounts for most of these deaths (17.9 million annually), followed by cancer (9.3 million). The WHO has set targets for noncommunicable diseases to be met by 2025 but the evidence in today’s report suggests that, across ESC member countries, most goals relating to heart health are unlikely to be achieved. For example, the WHO has called for a halt (with reference to 2010) to the rise in obesity. But between 2010 and 2016, the prevalence of obesity rose from 20.4% to 22.7% in women and from 19.2% to 22.2% in men.
Healthcare professionals will need to be properly trained to deal with the ever-increasing strain of this problem.
Read More