
High-fat diet can result in cognitive decline
A high fat diet can stimulate our immune cells to interfere with the connections between our neurones in our brain, known as synapses. This is the result of a study, originating in Georgia, USA that found that obesity causes chronic inflammation which in turn causes cells, known as microglia, in the brain to initiate an autoimmune response. Microglia are phagocytic cells that help the body’s immune system by fighting infectious agents in the brain but also are involved in the normal process of ‘synaptic stripping’. However in obesity they become activated and start to destroy the synapses instead. This study was conducted in two groups of mice that were given foods to mimic what a healthy diet and a fast food diet is like for humans. They found that after consuming a high fat diet, the mice recorded a lower level of activity in their hippocampus, the centre of learning and memory, which was due to the loss in synapses.
Thankfully, a low-fat diet of two months has been shown to reverse the effects of the autoimmune response, in mice. This brings hope not only to obesity sufferers but also to those with autoimmune diseases like Rheumatoid Arthritis as they are gaining more of an understanding of the impact of the inflammatory process on cells such as the microglia.
Read More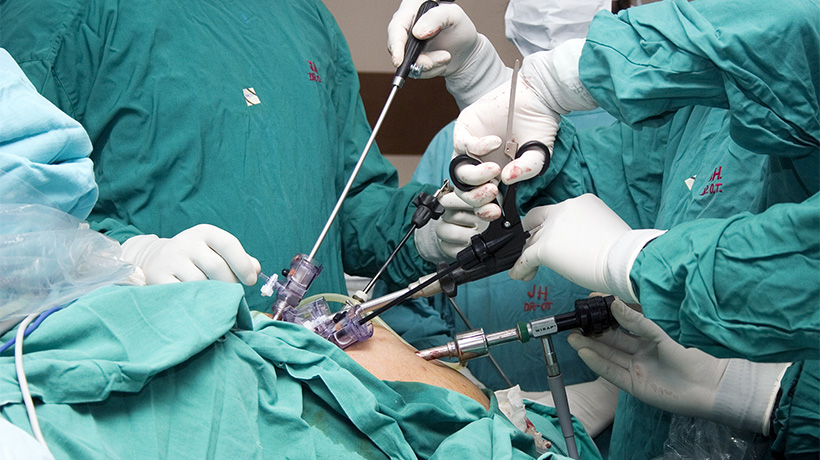
Bariatric surgery alters your food cravings
A new study claims that weight loss surgery can alter the reward pathways in your brain and therefore limit your sugar intake. Patients often report a change in food preferences after they undergo bariatric surgery, but clinicians have never really been sure why. The researchers aimed to build on prior knowledge that dopamine release can drive sugar cravings, whilst nutrient sensing in particular segments of the gut stimulates dopamine release. The researchers found that gastric bypass surgery in mice, the equivalent of the Roux-en-Y bypass in humans, resulted in less sugar-seeking behaviour by reducing the release of dopamine, which is heavily involved in reward systems.
The study suggests novel interventions that are less invasive and just focus on drugs that can reduce sugar cravings by targeting this pathway. More research needs to be conducted in order to find out if these effects are reproducible in other bypass surgery techniques. Furthermore, the results can create the basis of comparisons between different types of bariatric surgeries and how they each affect a patient’s behaviour.
Read More
The more fat you have, the harder it is to burn fat
The more fat you have, the more your body produces a protein that inhibits the ability to burn fat. An international team of researchers have published a study in Nature Communication that suggests a protein called sLR11 acts to suppress the process of thermogenesis. This is the mechanism by which brown fat cells keep us warm and ‘burn fat’. Using mice models, the researchers were able to switch off the gene which codes for this protein. Mice, as well as humans, increase their metabolic activity when switched to a high calorie diet, this means that they burn calories faster. However these mice without the gene responded with a much greater increase in metabolism, and were subsequently able to lose more weight.
The study looked at data from 1.2 million births from 2003 to 2011, which included 5,530 infant deaths (defined as a death before the first birthday). They also found that levels of sLR11 in the human body correlated with levels of total fat mass. The study brings hope to the use of thermogenesis as a target for obesity therapy, and related co- morbidities. This is because thermogenesis, when controlled properly, offers a way of disposing of fat in a relatively safe manner. The study also sheds light on the problem of many overweight individuals not being able to lose weight, as they have more sLR11, and therefore store more fat rather than burning it.
To learn more about obesity, its prevention, and its treatment please look at CCH’s Postgraduate Academic Courses in Lifestyle Medicine (Obesity Care), and CPD Short Courses in topics such as childhood obesity and behaviour change, designed to up-skill health professionals in this vitally important, and often overlooked, area of care.
Read More
Weight loss BEFORE pregnancy can reduce infant death
Being a healthy weight before being pregnant, whilst gaining an appropriate amount of weight during pregnancy, reduces the risk of the baby dying in its first year. This comes from a study by the Pittsburgh Graduate School of Public Health that explored the effect of weight counselling in women of a reproductive age. Dr Lisa Bodnar explained that ‘a third of women begin their pregnancy at an unhealthy weight, whilst over half gain too much or too little during pregnancy’.
The study looked at data from 1.2 million births from 2003 to 2011, which included 5,530 infant deaths (defined as a death before the first birthday). They found that in all weight classes, other than severely obese, gaining less than, or more than, the recommended weight increased the risk of infant death. However, even those that were obese and lost weight for their pregnancy were found to have twice the risk of infant death. However the study showed that it was much safer to lose weight before becoming pregnant, in order to reduce the risk of infant death.
Read More
‘Healthy diet’ is not the same for everyone
The way we metabolise foods differs from person to person, and one recent study is backing the idea of ‘personalised nutrition’. The study looked at the blood glucose levels of 800 people that consumed the same meals for a week. It is known that high blood glucose levels have a close association with obesity, pre-diabetes and Type 2 diabetes. The glycaemic index (GI) is normally used to rank foods on how they affect blood sugar levels. However, this study suggests that the effects differ from person to person.
Although many factors may affect the glucose response, they found that some individuals had vastly different responses to food, and some even in the opposite direction. This highlights the fact that, although some recommendations on dietary intake can be made, they can actually be detrimental to some patients. In order to discover why such vast differences may occur between people, the researchers analysed stool samples and came to the conclusion that gut bacteria play a major role in the responses for each person. They then adjusted meals for some patients, according to their previous responses, and were able to reduce post-meal spikes in blood sugar. To this end, it seems that personalised nutrition needs to be a reality soon in order to curb obesity epidemics and provide effective interventions for those affected.
To learn more about obesity, its prevention, and its treatment please look at CCH’s Postgraduate Academic Courses in Lifestyle Medicine (Obesity Care), and CPD Short Courses in topics such as childhood obesity and behaviour change, designed to up-skill health professionals in this vitally important, and often overlooked, area of care.
Read More