Use the code MTM50 at check out to save 50% this Black Friday ONLY!
Please Note: Offer ends Saturday 26 November 2016.

As the global obesity epidemic continues to escalate, different solutions are put forward every day by governments, private organisations, charities, and members of the public. Of the many varying solutions that are suggested, one, in particular, seems to have gained a lot of traction in the last couple of years; cooking classes. It is said that due to the obesogenic environment we live in, and both the stresses and conveniences of modern life, that the art of cooking, is a dying one. Time constraints and modern conveniences have seen a surge in the consumption of highly processed, high calorie, energy-dense food, and a plummet in people taking the time to cook, exercise and take part in other physical activity.
The argument for cooking classes is the idea that it will bring the public back into the kitchen where they will rekindle their love for fresh, healthy ingredients and homemade taste, whilst also getting more physical activity in the process. Cooking classes as a treatment for individuals with overweight and obesity is not a new idea, and has actually been in existence since early 2017 when the National Institute for Health and Care Excellence (NICE), and the NHS Diabetes Prevention Programme: Healthier You, both published guidelines suggesting, amongst other things, that cooking classes should be an option for those who are seeking to make drastic lifestyle changes in order to help treat, and even reverse, their obesity.
Adult cooking classes for individuals with overweight and obesity seem like a good idea, but that doesn’t mean it wasn’t greeted with its fair share of scepticism with Guardian columnist, Hugh Muir, stating “Cookery courses for obese people are pointless, and ministers know it.” Mr. Muir believes that cooking is no solution to the obesity crisis and that instead, it is government intervention and policy that should be the solution. What he fails to realise is that there is no single solution to such a complex problem and that government intervention, cooking classes, and a host of other obesity prevention initiatives are the answer.
Cooking classes have not just been recommended as a treatment strategy for adults with overweight or obesity, but also as a part of the preventative strategy for children as well. Many children growing up in the 21st Century have been surrounded by cheap takeaways and ready-made, or frozen, meals which have contributed to the rise of childhood obesity levels to unprecedented highs, and has left some children incapable of preparing any type of fresh meal. This includes every step of the process, from buying the raw ingredients at the supermarket, to preparation, and to finally cooking it. The idea was first proposed in the UK in 2008 by then Schools and Children Secretary, Ed Balls. He said, “Teaching kids to cook healthy meals is an important way schools can help produce healthy adults.” Eating habits, and education on nutrition, are certainly vital and necessary skills that our young people should be equipped with if they are ever to have a chance of remaining a healthy weight in our present environment.
Both Muir and Balls had very strong opinions on the helpfulness of cooking classes in the face of the obesity epidemic, but, neither had any evidence to help strengthen their positions at the time. Despite the scepticism, cooking classes have provided promising results as released for the first time this week by the NHS. Their diabetes prevention programme, Healthier You, introduced cooking to adults with obesity as part of a treatment plan and it was found that, “overweight people who attended NHS exercise and cookery classes lose an average of half a stone” Despite these results only being preliminary, it is certainly promising news for the fight in the obesity epidemic, and a great tool for helping us to reshape the way in which we can think about tackling it.
What’s important to remember, however, is that cooking classes will only truly be useful to the public if they have a professional help them understand the nutrition behind the meal they are preparing. However, given the level of nutritional education in current medical training, that will be a tall order. According to recent research, there is a “severe deficiency in nutrition education at all levels of medical training.” The foundational links between nutrition and weight management need to be understood by health professionals if we are to be serious about reversing the current worrying trends of overweight and obesity with the public. The College of Contemporary Health’s Nutrition and Weight Management short course was designed specifically to help rectify the lack of nutritional education that our healthcare professionals need. Cooking classes and health professionals with more robust and up-to-date nutritional education, together can take the public fight against the obesity epidemic a step in the right direction.
Read More
Smoking. Everyone knows the risks involved and the impacts it can have on your overall health. The links between smoking and emphysema, coronary heart disease, and in particular, cancer, have been long established and well publicised for decades. It is the biggest cause of preventable cancer cases in the UK, but perhaps what isn’t as widely known, and in this case, accepted, is what comes as a close second to smoking, and that is obesity. According to Cancer Research UK, “it’s thought that more than 1 in 20 cancers in the UK are linked to being overweight or obese,” and what is even more alarming is how little the public is aware of this fact with the same charity also stating that “being obese or overweight is linked to 13 different types of cancer, but only 15% of people in the UK are aware of the connection.”
Cancer Research UK took it upon themselves last week to inform the public of this health epidemic with a hard-hitting campaign that has been published on billboards and advertising space all over London and the rest of the UK. The campaign, designed in a “hangman game” style format, had the word obesity written in large font with letters missing from the word in order to make the public think, and guess, for themselves as to what the full word might be. What made the campaign especially hard-hitting is that it was designed in the exact same format found on cigarette packets which plainly details the, often gruesome, health risks involved with smoking. Using this format was an excellent way to effectively demonstrate that smoking and obesity can be as potentially dangerous as each other in causing cancer, and in both cases, lifestyle changes can be an effective preventative measure for developing the disease.

Cancer Research UK campaign advertisement seen in Peckham, London.
As the campaign made its physical presence felt, filling bus stops, tube stations, and various other advertising spaces around the UK, a quite unexpected backlash took hold on social media and discontent was soon voiced, and in many cases, sheer outrage emerged. Perhaps the loudest voice among the discontented was Danish comedian, Sofie Hagen, who, amongst other things, deemed this campaign as “hate.” Ms Hagen posted a series of tweets highlighting her outrage at the bold campaign from Cancer Research UK.
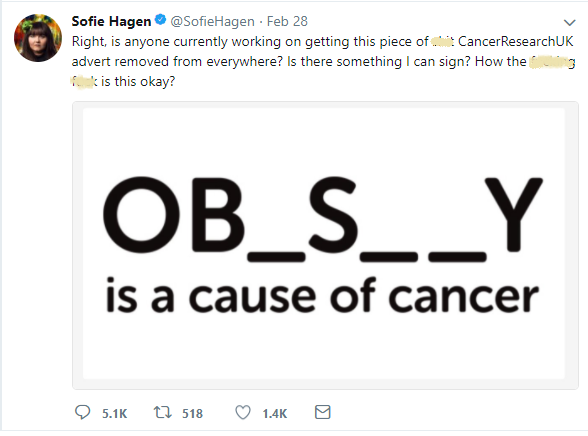
After imploring this campaign to be removed, even though it hadn’t even been present for a day, Ms. Hagen explained as to why she thought that it was so offensive and this was because, as she describes, “it uses shame, ridicule, abuse, and fear” in order to get individuals with overweight or obesity to “change their ways.” Many of Ms. Hagens followers agreed with her with one adding that “There is a difference between informing and shaming and THIS campaign shames.” Some were so enraged by Cancer Research UK’s campaign that they encouraged the public to never donate to the charity ever again and to only donate to charities that don’t body shame.
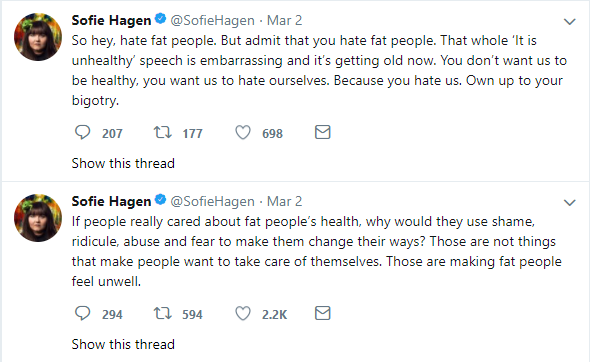
The outrage that this campaign attracted has drawn many questions, but one particularly pertinent question sticks out, and that is as to what exactly constitutes body shaming. Cancer Research UK’s campaign featured no people of any description in any of the variations of the advertisements. It only promoted the fact that after smoking, obesity is the biggest preventable cause of cancer, and was trying to make the public aware of this. So why was there such outrage? The outrage was probably due to the fact that obesity is an extremely sensitive topic and often the language used surrounding people with overweight or obesity is insensitive and counterproductive. There is no doubt that the way we talk about obesity needs improvement and should change, however attacking what is supposed to be an informing, and moving, campaign by a reputable national charity is not the way to do it.
The way to achieve a real change in the way we talk about obesity is to start using tools like People First language that the College of Contemporary Health was recently recognised for. People-First language is not something new; however, it is new to the obesity community. It separates the individual from their disease rather than labelling someone as their disease. For example, instead of using “the obese man was elderly” use, “the man with obesity was elderly.” People-First language, healthcare professionals trained in obesity care, and an awareness of obesity brought to the public by campaigns like this one by Cancer Research UK, is what will prompt real change in the way we perceive obesity in society and treat individuals with the disease.
To learn more about obesity, its prevention, and its treatment please look at CCH’s Postgraduate Academic Courses in Lifestyle Medicine (Obesity Care), and CPD Short Courses in topics such as childhood obesity and behaviour change, designed to up-skill health professionals in this vitally important, and often overlooked, area of care.

A group of MPs have urged the government that more must be done to reduce the number of multi-buy offers on unhealthy foods to help curb childhood obesity. Further to this, they say that rules on junk food advertising must get more stringent and clear, claiming that the current obesity plan set forth by the government is too vague. The British government announced a childhood obesity plan in 2016, one of the main points was the sugar tax, however many in the wider health community have criticised this plan saying that there must be more action.
In the latest Health Select Committee report, the MPs are calling for more to be done to stop big discounts on unhealthy food and therefore halt their promotion towards children. This comes after evidence from the food industry that responsible retailers are being undercut by those who continue to offer attractive discounts. Whilst some supermarket chains have reduced the number of deals that they promote, many others are still pushing theirs forward. The British Retail Consortium has stated that there will have to be industry-wide agreement if junk food promotions were to be reduced, and this is an incredibly difficult thing to implement.
The MPs also suggested that more must be done to stop junk food advertisements to children. Currently, these types of adverts are banned during programmes that are aimed at children, the MPs suggest that they should be banned during all programmes that children might watch as well. They go on to propose that the sugar tax should extend to milk-based products that are currently excluded but still contain added sugar. Whilst they are aware that many of these plans are ambitious, they are keen to point out that more must be done to stop the development of childhood obesity, and only by implementing new plans and strategies can this be achieved.
Read More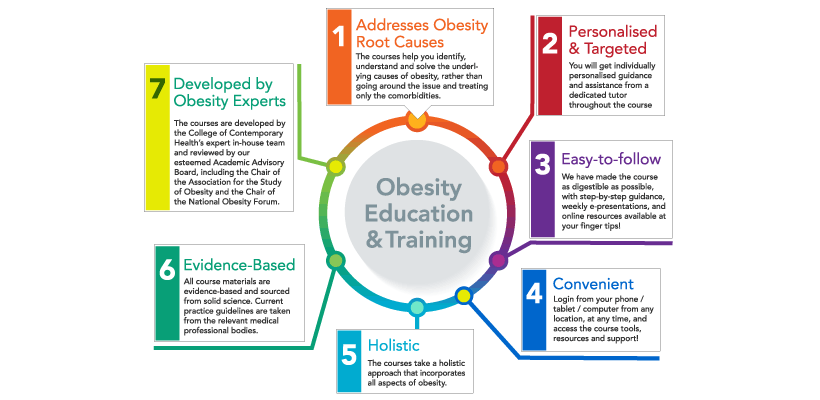
We have spoken quite a bit about the need for Obesity Education and Training.
Today, I would like to share with you the top 7 reasons some of our students chose to study Obesity Care and Management with CCH online.
Read More
This year’s 2016 Diabetes Professional Care conference was a hugely successful event. Held in London’s Kensington Olympia, many of the diabetic care industry innovators, specialists and thought leaders converged to share their knowledge and spread awareness of this increasingly prevalent and life-changing disease. The second ever instalment of this free-to-attend, CPD accredited exhibition included keynote presentations from NHS England and The Diabetes Think Tank, both of which were thoroughly engaging and informative, as well as many other presenters who demonstrated their passion and vision for the future of diabetes care.
When not attending one of the many talks or discussions over the course of the two days, attendees were given the opportunity to expose themselves to companies, their products, and representatives to get a feel for the field as a whole, covering the full diabetes spectrum from technologies, commissioning, diagnostics and prevention, to paediatrics, primary and secondary care. As well as being a great place for healthcare professionals to learn, the 2016 DPC provided a great chance to build invaluable relationships and network with those who share the same expertise and passion for diabetes care.
CCH made a great showing at the DPC and provided information to the attendees about the importance of education in the fight against diabetes and the best, and most compassionate, ways in which to care for patients. Although CCH is a fully online educational institute, it doesn’t mean we don’t relish the opportunity to meet so![IMG_4502[1]](https://www.contemporaryhealth.co.uk/wp-content/uploads/2015/03/IMG_45021-300x225.jpg) me of our students. Conferences like the 2016 DPC always attract the best and brightest in their field, so it’s no surprise to meet CCH students at an excellent event like this, and this year’s DPC provided us with the opportunity to meet CCH student, Dr. Sandhu. Dr. Sandhu is a GP based in Southall involved with many local charities, but what is most inspiring about her is her commitment to her continued pursuit of knowledge, and her ambition of achieving what’s best for her patients. She demonstrates how learning is something that continues throughout life, especially in today’s rapidly changing world.
me of our students. Conferences like the 2016 DPC always attract the best and brightest in their field, so it’s no surprise to meet CCH students at an excellent event like this, and this year’s DPC provided us with the opportunity to meet CCH student, Dr. Sandhu. Dr. Sandhu is a GP based in Southall involved with many local charities, but what is most inspiring about her is her commitment to her continued pursuit of knowledge, and her ambition of achieving what’s best for her patients. She demonstrates how learning is something that continues throughout life, especially in today’s rapidly changing world.
The great atmosphere and experience of the 2016 DPC will ensure that CCH will eagerly anticipate, and make a strong presence, at next year’s 2017 DPC! We hope to see you there!
Read More
Working with an overweight or obese client can be a daunting challenge. Most fitness professionals are ill-equipped to face the challenge head on because they’ve never been given the proper tools or understanding of their client’s situation. One of the biggest frustrations for your overweight and obese clients is not just losing the weight, but keeping it off once they’ve achieved that goal.
This globally accredited, 8-10 hour online course, prepares fitness professionals for the challenge of working with overweight and obese clients. It provides the tools and comprehensive knowledge required for fitness professionals to assist clients to successful weight-loss and weight-loss maintenance.
Fitness professionals can play a key role in the weight management of their clients; this course gives fitness professionals the confidence to workout and train with overweight and obese clients and significantly grow their client base.
All Making the Move: Working with Overweight Clientsstudents gain access to an extensive ‘fitness prescription toolkit’ that can be used immediately in client sessions.
Become certified in weight management with CCH
Please Note: Offer ends Saturday 26 November 2016.

According to ABC news, the average calorie intake at a Thanksgiving dinner is 4500 calories!
And, if you add your leftover turkey sandwich to the equation, that’s another 450 calories!
In order to burn off 85 calories you have to walk one mile at a brisk pace, so to burn off that incredible Thanksgiving feast, the drinks, and that left over turkey sandwich, you’ll have to walk 60 miles!
Don’t let that discourage you however, as Thanksgiving is a time to enjoy yourself and the company of your friends and family, and reflect on all you are thankful for.
From everyone at CCH, Happy Thanksgiving!

One in two adults currently living with diabetes is undiagnosed. This World Diabetes Day, the International Diabetes Federation are asking: individuals who may be at risk of type 2 diabetes, people living with diabetes, diabetes associations and health professionals to take action to help identify people with undiagnosed type 2 diabetes and those at risk of developing it in the future. The aim of identifying those at risk is to ensure early diagnosis, and therefore early treatment, of diabetes associated complications, such as blindness.
Read More

Diabetes is one of the fastest growing health threats in the UK, with over 4 million people living with the condition. With this figure only set to rise, the show offers healthcare professionals and practitioners the opportunity to update their knowledge of key suppliers, cutting edge technologies and solutions for the future of effective diabetes management, care and prevention.
CPD Accredited Conference Programme
Diabetes Professional Care will host a seven stream programme, covering the full diabetes spectrum from technologies diagnostics and prevention to commissioning, paediatrics and primary & secondary care.
 Visitors will, for the first time ever, be able to see Jonathan Valabhji, National Clinical Director for Obesity & Diabetes at NHS England and Dr Partha Kar, Associate National Clinical Director for Diabetes at NHS England take to the stage together, to present one of the show’s hotly anticipated keynote sessions. Valabhji will discuss ‘Diabetes and the NHS in England in November 2016’, while Kar will conclude by looking at ‘The art of the possible’.
Visitors will, for the first time ever, be able to see Jonathan Valabhji, National Clinical Director for Obesity & Diabetes at NHS England and Dr Partha Kar, Associate National Clinical Director for Diabetes at NHS England take to the stage together, to present one of the show’s hotly anticipated keynote sessions. Valabhji will discuss ‘Diabetes and the NHS in England in November 2016’, while Kar will conclude by looking at ‘The art of the possible’.
In a major show coup, Beverley Bryant, Director of Transformation at NHS Digital, will be discussing how new technologies are going to change the face of diabetes. Driven by the need to innovate, Bryant has been crucial in the movement towards making the NHS paperless, looking at the transformative powers that technology has to offer. For those who rely on technology or feel more faith should be put into it, this session is not to be missed.
Samantha Jones, Director, New Models of Care at NHS England will also be presenting on day one, analysing new models of care in diabetes, whilst Pauline Latham MP, Chair of the Diabetes Think Tank will feature in the afternoon session on day two.
|
To register for free entry to the conference and exhibition please visit www.diabetesprofessionalcare.com |
Dedicated Streams
Within the Primary and Secondary Care stream Debbie Hicks, Nurse Consultant – Diabetes from Enfield & Haringey Mental Health Trust & Co-chair – TREND-UK and Chair of FIT UK, will take a look at the learning curves experienced within diabetes care since the seventies. Hicks will also be running an interactive session on lipohypertrophy, which will see patients being treated live in one of the theatres, whilst educating visitors on how to identify this accumulation of fat underneath the surface of the skin, caused by multiple injections.
Dr David Haslam, GP and Chair of the National Obesity Forum, will be considering the scale of Diabetes in the UK and questioning how we should best address prevention.
Those interested in how technology can be used to combat diabetes, should look no further than the talk by the returning Dr Partha Kar. He will discuss ‘Diabetes & Technology: Overhyped or a necessity?’, while Sue Wales will continue with the theme, exploring how using innovations and technology can effectively improve diabetes control.
Exhibitors
As well as an action packed conference programme, Diabetes Professional Care 2016 has a wealth of innovative exhibitors signed up who will be sharing the very latest technologies and solutions, for the continued improvement and development of patient care in the diabetes field. This includes Hicom, Ascensia Diabetes Care, Cellnovo, Neuropad, Advanced Therapeutics, METEDA, Novo Nordisk, Siemens Healthineers, Abbott and Diasend.

Because LSBU are always keen to hear about the real impact LSBU is delivering with their partners, we’ve met with one of the first students enrolled on the course. Divya Bassi is a Macmillan Support Worker and is studying towards an MSc in Obesity Care and Management at CCH.
Hi Divya, thank you for taking the time to chat with us. Why the interest in obesity studies?
I currently work for the Macmillan South West Aftercare team. We offer long term specialist support and advice to childhood cancer survivors. Within clinic, we have a unique opportunity to work with patients to promote healthy lifestyle choices to improve overall health and wellbeing. This cohort can encounter other health care issues as a result of their treatment which can be further perpetuated by an unhealthy lifestyle. Maintaining a healthy weight is crucial, and obesity prevention is an area I feel particularly passionate about.
I feel that the learning from this course fed directly into improving my practice with patients. It offered me the opportunity to liaise with other health care professionals within weight management and also presented practical strategies that covered the holistic management of this complex healthcare issue.
And why did you choose the CCH?
To my knowledge, this institution was the only one that offered Master’s level work in obesity management via distance learning.
So, what did you think of the online format?
The online format is easy to use and enables the user to control their learning. I could access the forum when convenient for me and around my other professional / social commitments. There was always someone available to help if I came across any issues with the platform and there was a wide range of resources available to support my learning.
Do you feel the course helped to improve your practice with patients?
Absolutely. I feel that the learning from this course fed directly into improving my practice with patients. It offered me the opportunity to liaise with other health care professionals within weight management and also presented practical strategies that covered the holistic management of this complex healthcare issue.
Would you recommend the course and CCH?
Yes, I would definitely recommend the course to other professionals within obesity management. The flexible format and opportunity to share learning with other professionals was great. Working with patients around their weight management is complex, and the training that I have received through CCH has been invaluable.
Lastly, before you go, what is your mission as a healthcare professional?
I feel passionate about endorsing a holistic approach to the current obesity epidemic which utilises a range of strategies around a patient centred approach. In my experience, considering all of the multi-factorial triggers that can contribute to weight gain is key. I strive to continue learning within this area of expertise so that I can support patients in the best way possible to achieve successful behaviour change. I also feel strongly about the need for more preventative strategies around weight management, especially for the younger generations. The healthier choice should be the easy choice, and I hope to contribute to the continued mission to prevent obesity in children and young people.

On the 14th July 2016, Pokémon Go™ was released in the UK. The App relates to the animated game Pokémon™, that allows users to capture different characters and complete challenges. It is made explicit to the user when downloading the App that they will need to be physically active to engage with the game.
Researchers from the Academy of Sport and Physical Activity at Sheffield Hallam University are studying whether the Pokémon Go™ App has increased physical activity in the last 7 days.
The research team are recruiting people aged 18 years and older from across the world to complete an online survey. If you would like to complete the survey or for more information, please follow the link below:
https://shusls.eu.qualtrics.com/SE/?SID=SV_4Git5qVSH4ZA1al
Read More
 I wanted to attain a qualification that would help me secure employment in the field of obesity management. The College of Contemporary Health was the only institution able to offer me the depth of course that I was looking for as well as the ability to study at a distance.
I wanted to attain a qualification that would help me secure employment in the field of obesity management. The College of Contemporary Health was the only institution able to offer me the depth of course that I was looking for as well as the ability to study at a distance.
 The resources are great. Interesting podcasts/videos and it’s nice to have the links available for the required reading.
The resources are great. Interesting podcasts/videos and it’s nice to have the links available for the required reading.
 The course has been extremely interesting. A lot of work has clearly been put in to making it informative, challenging and thought provoking. The online format works well for me as I can fit my studies in around my other commitments. The use of the discussion forums has allowed me to have interactions with other students and get their opinions and feedback. It is valuable that all the students come from different sectors, so that we get a more holistic view of obesity care. It also means that even though you are studying alone, you feel as though you are part of a class.
The course has been extremely interesting. A lot of work has clearly been put in to making it informative, challenging and thought provoking. The online format works well for me as I can fit my studies in around my other commitments. The use of the discussion forums has allowed me to have interactions with other students and get their opinions and feedback. It is valuable that all the students come from different sectors, so that we get a more holistic view of obesity care. It also means that even though you are studying alone, you feel as though you are part of a class.
 My course tutor is incredibly hardworking, he makes himself accessible on days and during hours I believe that most would not, and this is greatly appreciated as it allows me to work around my personal schedule.
My course tutor is incredibly hardworking, he makes himself accessible on days and during hours I believe that most would not, and this is greatly appreciated as it allows me to work around my personal schedule. Very well presented. I liked the fact that it was delivered -weekly as it kept my momentum up and I did not feel overwhelmed. It has been extremely informative, and I am thoroughly enjoying learning.
Very well presented. I liked the fact that it was delivered -weekly as it kept my momentum up and I did not feel overwhelmed. It has been extremely informative, and I am thoroughly enjoying learning.
 We are absolutely thrilled to be working in partnership with the College of Contemporary Health on such an innovative and progressive project.
We are absolutely thrilled to be working in partnership with the College of Contemporary Health on such an innovative and progressive project.Read More
