
Personalised Care Institute launches VR training for shared decision making
The Personalised Care Institute (PCI) has recently launched virtual reality training on shared decision-making (SDM) to help healthcare professionals fill gaps in their knowledge, which they have reported. This training, commissioned by NHS England, aims to explore key micro-skills around shared decision-making, including agenda setting, teach-back, exploring patient preferences, and reaching a shared decision. By practising these skills in a risk-free virtual environment, healthcare staff can improve and develop their skills for the benefit of their patients.
Shared decision-making has been shown to result in better patient outcomes, with increased adherence to treatment, fewer repeat appointments, and fewer regrets about decisions made over their health and care. However, 46% of healthcare professionals report gaps in their knowledge on the topic, according to The Patient Association, and 70% of them want to learn more.
The Personalised Care Institute developed a free, quality-assured eLearning tool called Virtual Patient Simulation: Test Your Personalised Care Conversations in conjunction with Keele University. This tool allows users to put their shared decision-making skills to the test through a series of life-like simulated patient consultations. It uses multiple-choice questions to provide a structured interaction with an on-screen animated patient character. Comprehensive feedback is delivered at the end of each exercise, allowing users to put what they’re learning to the test with repeated use.
Dr Emma Hyde, the clinical director of PCI, said that although research suggests only one in three healthcare professionals always practise shared decision-making fully, the perceived common barriers include lack of experience, confidence, and time. She believes that these could be quickly overcome with the opportunity to practise. “Not only will this training equip health and care professionals with the shared decision-making skills and knowledge needed to deliver the very best health outcomes for patients, but it will also address the growing desire among the general public for greater involvement in key decisions that inform their healthcare,” she added.
The use of simulations can help to encourage greater engagement and facilitate repetitive practice, and at the same time allows users to work at their own pace. Dr Priti Kadoo, a GP in frailty medicine and an ambassador for the PCI, said that the VR training helps professionals reflect on current practice and really think about personalised care and striking the right balance between imparting clinical information and considering how the patient feels and is likely to respond to what they tell or ask them.
The first scenarios launched are an in-person consultation based on an osteoarthritis discussion and a remote consultation by telephone with a father concerning his son’s sore throat. Two further scenarios – a referral for suspected bowel cancer and a discussion around the ongoing use of antidepressants – are due to be launched in the coming months.
The use of virtual reality to train healthcare professionals is becoming more widespread. Last year, Norfolk and Norwich University Hospitals NHS Foundation Trust introduced new virtual reality films for dementia education. The aim of the VR films was to help healthcare professionals gain a better understanding of the challenges patients living with dementia face when on a busy inpatient ward.
Read More
Using non-fungible tokens for secure health data management
SingHealth, a healthcare provider in Singapore, is exploring the use of non-fungible tokens (NFTs) as a potential solution for managing and exchanging health data in a secure and privacy-preserving manner.
NFTs, which are unique digital data units stored on the blockchain, offer features of uniqueness, transparency, and interoperability. Health data can be minted, exchanged and stored using blockchain technology, which would allow patients to own and exchange their personal health data with multiple stakeholders. Each patient can own, store and share their health data in the form of NFTs using a health wallet hosted on a secure web-based or smartphone application.
The use of NFTs shifts the onus of sharing individual patient data to each patient, thus fostering a closer relationship between the healthcare provider and the patient. Furthermore, sharing health data as NFTs ensures complete transparency and accuracy of healthcare research data, due to the traceable and unalterable nature of the blockchain.
SingHealth anticipates a growing need for privacy-preserving solutions to enhance the applications of data for medical research and clinical care purposes, and the use of NFTs will allow for a secure healthcare data exchange platform.
Read MoreHealth Education England publishes roadmap for use of AI in the NHS
Health Education England (HEE) has released the first-ever roadmap outlining the use of artificial intelligence (AI) in the UK’s National Health Service (NHS) and its impact on the healthcare workforce.
The report analyses the implementation of AI and data-driven technologies in the NHS, their adoption rate, and the impact on staff. The roadmap aims to provide insight to healthcare leaders into AI policy, education, regulation, innovation, digital transformation, and workforce strategy. The report examines the timeframe for AI projects’ implementation, the distribution of AI technology in clinical areas and the workforce, the different uses of AI in healthcare, and the effects on staff and patients.
Dr Hatim Abdulhussein, clinical lead for the Digital, Artificial Intelligence and Robotics Technologies in Education (DART-Ed) programme at HEE, states that the AI roadmap is a valuable asset in understanding the AI and data-driven healthcare landscape and its implications on staff and learners. The report is a collaborative effort between Unity Insights, NICE, NHS AI Lab, and the NHS Accelerated Access Collaborative (AAC). The report also builds on the Topol review, providing a framework to identify and classify AI technology in healthcare.
The report finds that diagnostic technology, such as those used in imaging, pathology, and endoscopy, accounts for the most significant proportion of AI use in healthcare (34% share), followed by automation/service efficiency, P4 medicine, remote monitoring, and therapeutic. Of the 56 technologies estimated for large-scale deployment within a year, 77% are for use in secondary care, 23% for use in primary care, and 7% for use in community care. A total of 155 workforce groups, across 67 clinical areas, use AI tech identified by HEE, with medics in clinical radiology and general practice being the most affected, as well as non-clinical admin staff.
Abdulhussein highlights the importance of achieving transformation through emerging technology to improve patient care and scalability throughout the country, and the roadmap’s insights will focus efforts on education and training. The UK government recently unveiled its ten-year national plan to tackle cancer, including an increased use of AI and machine learning in NHS healthcare. England is also trialling a new approach to the ethical adoption of AI in healthcare.
Read More
The Potential Role of Digital Health in Obesity Care
The journal Advances in Therapy has recently published a paper exploring the use of digital health technologies in improving obesity care.
Obesity is a complex and chronic condition that increases the risk of developing several diseases, including type 2 diabetes mellitus, cardiovascular disease, and certain cancers. The prevalence of obesity continues to rise and poses a significant economic burden on healthcare systems worldwide. Current obesity treatment approaches tend to focus on individual responsibility, diet, and exercise, but they fail to acknowledge the complexity of the condition and the need for a whole-system approach.
A new approach is necessary that recognises the complexity of obesity and offers patient-centred, multidisciplinary care tailored to the needs of each individual. Digital transformation can significantly benefit obesity treatment, particularly through telehealth and mobile health, which can provide improved support and monitoring of behaviour change. Furthermore, artificial intelligence (AI) can revolutionise obesity care by enabling real-time patient monitoring and personalised interventions.
Digital health technologies offer a range of potential benefits for people with obesity, including improved quality, efficiency, and cost-effectiveness of care at all stages, from patient assessment to treatment and ongoing monitoring and support. Telehealth and mobile health are already widely used in healthcare and can reduce barriers to effective obesity care, improve access to care, and ultimately improve long-term weight management and obesity-related health outcomes. However, equitable access to telehealth and mobile health services must be ensured for patients from the most deprived communities.
Machine learning and AI can play an increasingly important role in healthcare and provide several opportunities for obesity care. By analysing large datasets from electronic health records, healthcare professionals can enhance their understanding of obesity’s complexity, leading to improved patient assessment and personalised treatment. Additionally, AI can be applied to mobile health technologies, connected via the Internet of Medical Things, to provide real-time patient monitoring and personalised weight management interventions.
In the immediate future, the most significant digital advancement in obesity care is likely to be the increased use of telehealth support, allowing greater access to care, more frequent consultations, and longer-term support. Over time, this will increasingly be supported by mobile health apps and devices. Ultimately, interventions and ongoing support are likely to be delivered using AI technology through a chatbot or avatar.
Please read the full paper here: The Potential Role of Digital Health in Obesity Care
Read More
Smart data and population health can build better, healthier lives
In recent years, there has been growing interest in how population health management can help improve the lives of citizens. Here, we explore how machine learning can provide the data intelligence we need to deliver better healthcare for everyone.
Preventative healthcare is known to be more effective than reactive healthcare. By intervening early and preventing health issues from escalating, individuals, communities, and healthcare providers can all benefit from improved outcomes. With the UK healthcare system under immense pressure, there is a pressing need to shift towards a proactive approach. However, in order to achieve this, we need to understand what factors influence health outcomes. For example, why do people in one area have fewer healthy life years than those in another part of the country?
Population health intelligence is the discipline of finding answers to questions like this. By making the right interventions at the right time, we can improve health outcomes. As Integrated Care Systems (ICSs) work to tackle some of the NHS’s most pressing problems, such as health and care inequalities and financial sustainability, population health intelligence can help make the connections between health outcomes and the factors that influence them.
ICSs bring together NHS, local authority, and third sector bodies, providing access to all the data needed to gain a deeper understanding of population health. This includes everything from NHS records to data on education, housing, and crime. However, the challenge is how to extract the relevant insights that can point to new and better ways of doing things.
Data on life expectancy is a good starting point. It is also a sound measure of health inequality, which is currently in the spotlight. Unlike health data or patient reported outcome measures (PROMS), life expectancy data doesn’t depend on people having accessed healthcare, making it a more inclusive and accurate proxy for overall population health. The variations in the data are stark, with men and women born in Glasgow City today expected to live around 10 years less than those born in Westminster or Kensington & Chelsea.
To understand what’s behind these stats, machine learning can make meaningful analysis of disparate datasets. It can rapidly work across huge volumes and multiple sources of data to identify patterns that can guide decision-making. Population health intelligence can help us analyse the causes of death at different ages in different demographics and the wide range of influences on them.
Factors such as education and housing can affect health outcomes. For example, data analysis may connect high levels of poor housing stock with respiratory illness. This could ultimately show that making improvements to living conditions today could prevent people from developing chronic conditions that lead them to depend on multiple health and care services in the future.
In a similar way, information on dental health, such as the number of people in a single area having teeth removed at a young age, could also be a predictor of chronic conditions such as diabetes and heart disease in future life. This information could direct healthcare interventions towards support for diet and lifestyle changes.
By connecting health data with environmental information, such as air quality or the amount of available green space, population health intelligence techniques could show local authorities where to focus their investment, where people’s physical and mental wellbeing will benefit the most.
Health-related wearables also support the shift towards more personalised and proactive healthcare. From simple step counters and heart rate monitors to sophisticated continuous glucose monitors, people are increasingly willing and motivated to track their own wellbeing. When connected to healthcare systems and analysed by machine learning algorithms, wearable devices and apps could support preventive healthcare by alerting professionals to potential issues, for example, an individual showing pre-diabetic symptoms.
The UK’s move towards integrated care systems presents a huge opportunity to build a proactive approach to healthcare based on insights gleaned from many different data sources. Machine learning is vital for unlocking this potential, helping to build more innovative, impactful, and cost-effective healthcare.
Read More
AI could help predict medical conditions earlier thanks to unique health data sets
Nightingale Open Science, a project launched by Ziad Obermeyer, a physician and machine learning scientist at the University of California, Berkeley, offers a unique and free medical dataset aimed at solving medical mysteries through the use of artificial intelligence (AI).
The project, which was funded with $2 million from former Google CEO Eric Schmidt, consists of 40 terabytes of medical imagery such as X-rays, electrocardiogram waveforms, and pathology specimens from patients with various conditions, including Covid-19, sudden cardiac arrest, fractures, and high-risk breast cancer. Each image is labelled with the patient’s medical outcomes, such as the stage of breast cancer, whether it resulted in death, or whether a Covid-19 patient required a ventilator.
The datasets were curated with the help of hospitals in the US and Taiwan over a period of two years, and Obermeyer plans to expand this to include more medical diversity in Kenya and Lebanon in the coming months. The key differentiating factor between these datasets and those that are available online is that they are labelled with “ground truth,” meaning that they are based on what actually happened to the patient rather than a doctor’s opinion.
The AI community has recently shifted its focus from collecting “big data” to more meaningful data, which is relevant to a specific problem and can be used to address issues such as inherent biases in healthcare, image recognition, or natural language processing. In healthcare, algorithms have been shown to amplify existing health disparities. For example, an AI system used by hospitals to allocate additional medical support for patients with chronic illnesses was found to be prioritising healthier white patients over sicker black patients who needed help, due to the use of healthcare costs as a proxy for healthcare needs.
The Nightingale Open Science project is aimed at producing high-quality datasets that are more representative of the population and can be used to root out underlying biases that are discriminatory towards underserved and underrepresented groups in healthcare systems, such as women and minorities. These diverse datasets can also help to study the spread of diseases in different cultures and locations, where people may react differently to illnesses.
The availability of high-quality, diverse medical datasets can enable AI to predict medical conditions earlier, triage better, and ultimately save lives. The Nightingale Open Science project, which provides unique and curated datasets based on actual patient outcomes, has the potential to drive progress in healthcare and reduce the impact of biases on healthcare systems.
Read More
AI could save the healthcare industry up to $360B a year
The ChatGPT AI model is generating a buzz in healthcare as it has passed the U.S. medical licensing exam, authored scientific papers, and is being used to appeal insurance denials. However, despite research indicating the benefits of AI in healthcare, actual adoption of AI-based tools remains low.
In a new paper, researchers estimate that broader adoption of AI in healthcare could result in savings of between 5% and 10%, or roughly $200 billion to $360 billion a year. These savings could be achieved by using AI for use cases that employ current technologies attainable within the next five years, without sacrificing quality or access.
For hospitals, AI could bring cost savings by improving clinical operations, quality, and safety, such as optimising operating rooms or detecting adverse events. Physician groups could use AI for continuity of care, like referral management. Health insurers would see savings from use cases that improve claims management, like automating prior authorisation, along with healthcare and provider relationship management, including preventing readmissions and provider directory management.
Based on AI-driven use cases, private payers could save around 7% to 9% of their total costs, amounting to $80 billion to $110 billion in annual savings within the next five years. Physician groups could save 3% to 8% of costs, amounting to between $20 billion and $60 billion in savings. Hospitals could see savings between 4% to 11%, or between $60 billion and $120 billion each year, according to the report’s estimates.
While the potential benefits of AI in healthcare are significant, and the Food and Drug Administration has accelerated approvals of medical AI tools, actual adoption remains hit-or-miss. A recent study published in JAMA found a “paucity of robust evidence” to support claims that AI could enhance clinical outcomes. However, experts believe 2023 could be a turning point for adoption as more evidence around AI’s efficacy in real-world settings emerges.
Read More
PGCert, PGDip, and MSc in Digital Health launched
The College of Contemporary Health (CCH) has been involved with the development of University of Central Lancashire’s (UCLan) new postgraduate programme in Digital Health. The programme, Master of Science (MSc) in Digital Health, is designed to provide students with a comprehensive education in the use of technology in healthcare. The flexible design enables the student to exit the programme with either a Postgraduate Certificate (PGCert), or a Postgraduate Diploma (PGDip) in digital health.
The programmes will cover key areas such as telemedicine, artificial intelligence, and the use of wearables in healthcare. Students will have the opportunity to develop a deep understanding of the ways in which digital technologies can improve the delivery of care and enhance patient outcomes. The coursework will be delivered by experienced professionals from the healthcare and technology industries, providing students with a unique blend of academic and practical expertise.
The MSc programme is aimed at doctors, healthcare professionals, and other individuals who wish to specialise in digital health. The PGCert and PGDip programmes are designed for those who want to develop a more general understanding of the field and gain a solid foundation in the use of technology in healthcare.
The launch of these new programmes reflects CCH’s commitment to providing high-quality education and training in digital health. CCH aims to equip students with the skills and knowledge they need to make a positive impact in the field of digital healthcare, an exciting and rapidly developing field that will present graduates with a vast array of opportunities going forward.
All awards will be awarded by the University of Central Lancashire (UCLan).
Read More
UK and Ireland collaborate for innovation in Digital Health
Ireland and the United Kingdom recently announced a new collaboration aimed at promoting digital innovation in the healthcare sector. The partnership aims to bring together the expertise and resources of both countries in order to create new, cutting-edge solutions for the delivery of healthcare services.
One of the key goals of this collaboration is to develop new digital technologies that can help improve patient outcomes and experiences. This will be achieved through the creation of innovative digital tools and platforms that can help healthcare providers to better manage patient care, as well as through the development of new approaches to medical research and development.
Another important aspect of this collaboration is the sharing of best practices and knowledge between healthcare providers in both Ireland and the UK. This will help to ensure that healthcare providers in both countries are able to stay up-to-date with the latest developments and advancements in digital health.
The collaboration will also focus on the creation of new business opportunities in the digital health sector. This will include the development of new products and services that can help to improve the delivery of healthcare, as well as the creation of new start-ups and spin-off companies that can bring innovative solutions to the market.
Overall, the collaboration between Ireland and the UK is expected to have a positive impact on the healthcare sector, both in terms of patient outcomes and in terms of the growth of the digital health industry. By working together, the two countries hope to establish themselves as leading players in the digital health space and to drive forward innovation and progress in the field.
The partnership is a significant step forward in the ongoing effort to modernise the healthcare sector and to make healthcare services more accessible, efficient, and effective for patients. With the collaboration between Ireland and the UK, we can expect to see a range of new digital health solutions emerging in the coming years, which will help to improve the lives of patients and healthcare providers alike.
Read More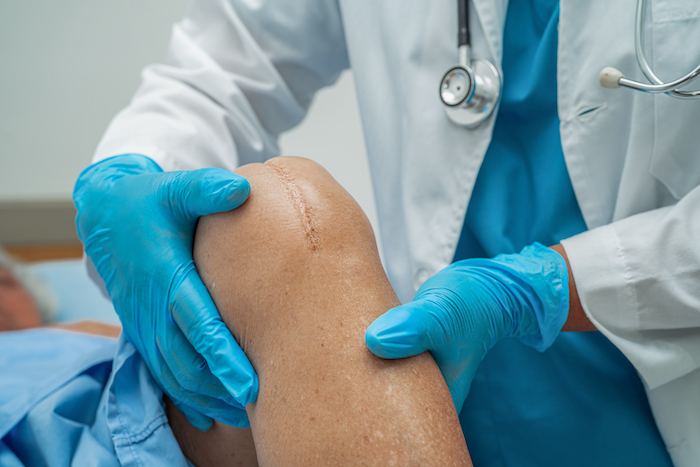
Telehealth programs improve outcomes in patients with knee osteoarthritis, obesity
Telehealth programs have shown to positively impact patients with knee osteoarthritis and obesity. A recent study found that these programs improve patient outcomes by providing convenient access to care, increasing patient engagement and promoting lifestyle changes. The study participants using telehealth reported higher levels of physical activity and better overall knee function compared to those who did not use telehealth. The findings highlight the potential for telehealth to improve the management of chronic conditions and the delivery of care for patients. The results also demonstrate the importance of technology in healthcare, as telehealth programs can bridge gaps in access to care and support better patient outcomes.
Read More
AI chatbots could help patients discuss sensitive health conditions
Artificial Intelligence (AI) technology, specifically chatbots, have the potential to help patients with sensitive health conditions, according to a recent article from Digital Health. Chatbots can provide quick and easily accessible information, support, and guidance to patients, especially those with sensitive health conditions that require constant monitoring and care.
One of the key benefits of chatbots in healthcare is their ability to provide quick and accurate information to patients. Chatbots can answer patients’ questions, provide them with educational materials, and even schedule appointments, freeing up time for healthcare professionals to focus on more complex tasks.
For patients with sensitive health conditions, chatbots can provide emotional support and help manage symptoms. Chatbots can engage in conversations with patients, listen to their concerns, and provide them with coping strategies and resources. This can improve the patient’s overall well-being and help them feel more in control of their health journey.
Chatbots can also assist in monitoring patients’ health status and provide real-time feedback. For example, chatbots can remind patients to take their medications, track their symptoms, and even provide alerts to healthcare professionals if there are any concerning changes in the patient’s condition.
From providing quick and accurate information, to offering emotional support and monitoring health status, chatbots have the potential to play a significant role in the care of patients with sensitive health conditions and can improve the overall experience for patients enhancing the quality of care they receive.
Read More
Minister praises Saudi Arabia’s use of digital health in virus fight
The adoption of digital health technologies as new standards in Saudi Arabia reflects the country’s leadership in international and regional forums, according to Saudi Health Minister and Chairman of the Saudi Health Council, Fahad Al-Jalajel. In his speech at the opening of the HIMSS21 Middle East Health Conference, Al-Jalajel emphasised the crucial role digital technologies played in dealing with the COVID-19 pandemic. The first interactive map of COVID-19 data was launched to provide accurate statistics and employ artificial intelligence to analyse the data and make national strategic decisions.
The HIMSS21 conference aims to discuss current challenges and exchange ideas and experiences in the field of healthcare, both regionally and internationally. The conference will also highlight the importance of health information technology and its role in improving the efficiency of performance, enhancing the quality of services, and optimising the use of resources.
Innovative plans are being implemented in Saudi Arabia to develop the health system, including building a health transformation plan and designing programs for governing, financing, and providing health services. Digital health is a critical partner in this transformation, in line with the National Transformation Program and the country’s Vision 2030.
Secretary-General of the Saudi Health Council, Dr. Nahar Al-Azmi, stated that the HIMSS21 conference will also address the current challenges in the health sector and propose visions and ideas for future plans and potential solutions. The conference will provide an opportunity for exchanging knowledge, experiences, and expertise, as well as global dialogues on the challenges facing health systems and the available solutions. The goal is to harness digital health to build effective responses to future epidemics, benefit from data and technology to enhance population health management, and adopt digital health technologies as new standards to improve the quality of healthcare.
Read More