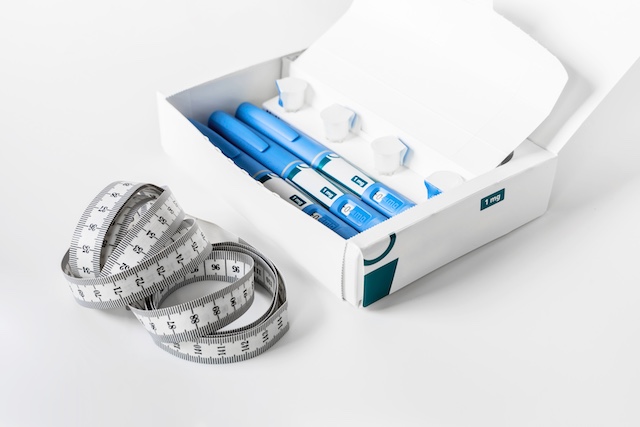
Britain’s drug regulator approves Novo Nordisk’s weight loss drug Wegovy to cut heart disease risk in patients with obesity
On Tuesday, the 23rd of July, 2024, the United Kingdom’s Medicines and Healthcare products Regulatory Agency (MHRA) granted approval for an additional use of Novo Nordisk drug, semaglutide (marketed as Wegovy), targeting the reduction of cardiovascular risks in adults with overweight and obesity.
Originally sanctioned for obesity treatment and weight management in conjunction with dietary, physical, and behavioural interventions, semaglutide, a GLP-1 receptor agonist, has now emerged as the pioneering prescription weight loss medication to thwart cardiovascular incidents. This includes the prevention of cardiovascular death, non-fatal myocardial infarction, and non-fatal stroke in individuals possessing a Body Mass Index (BMI) of at least 27 kg/m2 who already suffer from established cardiovascular disorders.
The endorsement by MHRA is supported by recent data derived from a post-approval clinical trial, indicating that a weekly subcutaneous injection of semaglutide (2.4 mg) over a span of up to five years considerably diminishes the occurrence of major adverse cardiovascular events (MACE) when compared to a placebo.
In a significant international study, which randomly allocated more than 17,600 participants to either receive Wegovy or a placebo, the treatment with Wegovy was observed to reduce the risk of major adverse cardiovascular events by 20%. These events transpired in only 6.5% of the Wegovy group, as opposed to 8% among those who received the placebo.
Recent research underscores the efficacy of semaglutide in augmenting the life quality of individuals with cardiovascular diseases by substantially lowering the risk of severe cardiac episodes.
Furthermore, in a strategic expansion move, Novo Nordisk procured a 200-acre plot earlier this month in Odense, Denmark’s third-largest city. The company has initiated preliminary excavation activities at this site, potentially setting the stage for a new manufacturing facility.
The surge in demand has propelled the pharmaceutical giant to invest billions in amplifying its production capacities in both Denmark and the United States. While the specific purpose of the new site in Odense remains to be officially confirmed, a report by Reuters in January highlighted that the site might accommodate facilities crucial for the fill-finish process involved in injection pen manufacturing.
A company statement released to Reuters mentioned, “With the political processes and approvals in place, we are pleased to announce that Novo Nordisk is now the owner of the site in Tietgenbyen in Odense.”
The company further indicated that the decision-making process regarding the precise use of the new site would conclude by the end of the year, post-internal approvals. The environmental report sheds light on future plans, which include establishing a packaging facility by 2026 and a factory for moulding plastic components necessary for pen and possibly tablet production by 2030.
Read More
Nutritional studies highlight pulses as key to lowering diabetes and cholesterol risks
Research consistently highlights pulses—such as beans, peas, lentils, and chickpeas—as crucial allies in the fight against diabetes and elevated cholesterol levels. This insight comes at a critical time, as projections from a study published in The Lancet last year forecast that diabetes could affect over 1.31 billion people globally by 2050. Concurrently, elevated cholesterol levels remain a significant health issue, with nearly half of adults in the UK exceeding national guidelines.
A detailed review in the journal Nutrients has shown that regular consumption of pulses can significantly improve these concerning health trends. The review meticulously examined thirty studies that looked at various types of pulses, including lentils, chickpeas, and several common beans like pinto, black, and kidney beans. The studies covered a wide array of health outcomes, from lipid profiles and blood pressure to risks of cardiovascular diseases and diabetes management.
The findings from these studies are telling. They specifically note improvements in low-density lipoprotein (LDL) and high-density lipoprotein (HDL) cholesterol, systolic and diastolic blood pressure, fasting blood sugar, haemoglobin A1c levels, waist circumference, and markers of inflammation and sensitivity such as C-reactive protein. These outcomes particularly underscore the potential of pulses to enhance lipid profiles and manage blood pressure.
The review emphasised that interventional studies, which typically have larger sample sizes and provide robust data, consistently confirm the health benefits of pulses. These studies often involved dietary adjustments where pulses replaced red meat or were added to diets as fixed servings. The results repeatedly demonstrated improvements in dietary quality and beneficial health outcomes.
Pulses’ potential to prevent heart disease is particularly noteworthy, largely due to their ability to lower total and LDL cholesterol levels. The authors of the review highlight that pulses are low in fat and rich in healthy mono- and polyunsaturated fats, essential micronutrients, and bioactive compounds with antioxidant properties, making them a true “nutritional powerhouse.”
Longitudinal studies also link higher pulse consumption with reduced risks of developing type 2 diabetes. This association is bolstered by interventional studies that document notable improvements in fasting glucose levels and insulin sensitivity with increased pulse intake. Consequently, pulses are not only pivotal in preventing diabetes but also in managing blood glucose levels effectively.
Tim McGreevy, CEO of USA Pulses, commented on the research, stating, “This research accentuates the fact that pulses are beneficial for health in so many ways, underscoring dietary guidelines that endorse plant-based eating patterns,” even though he was not directly involved in the study.
Additionally, awareness about type 2 diabetes is critical as many individuals may be unknowingly afflicted. Symptoms to watch for include increased urination, persistent thirst, excessive tiredness, unexplained weight loss, genital itching or recurrent thrush, delayed healing of wounds, and blurred vision. Recognising these signs can prompt earlier intervention and management of the condition, further reducing long-term health risks.
Read More
Lifestyle changes in mothers with obesity could mitigate heart risks in offspring
Researchers at King’s College London have discovered that lifestyle modifications could potentially reduce the risk of children developing certain cardiovascular diseases, which are believed to stem from maternal obesity and related foetal heart abnormalities.
Globally, obesity rates among pregnant women are on the rise, with more than half of the women attending antenatal clinics in England and Wales either having overweight (28.5%) or obesity (22.7%). Studies have increasingly shown that obesity during pregnancy can precipitate cardiovascular complications and disrupt normal cardiac development in the offspring.
The findings were detailed in a recent publication in the International Journal of Obesity, led by Dr Samuel Burden. The research team conducted a systematic review of existing studies to explore whether interventions targeting obesity in pregnant women—through diet, exercise, and other physical activities—can foster cardiac health in their children.
The selection criteria for the studies included randomised trials focusing on lifestyle changes among pregnant women diagnosed with obesity. The evidence reviewed indicated that such interventions could avert atypical cardiac development in children, highlighting several benefits commonly associated with improved heart health, such as decreased thickening of the heart walls, maintaining normal heart weight, and reducing the likelihood of increased heart rates.
Dr Samuel Burden commented, “We and others have demonstrated that maternal obesity correlates with signs of poor heart development in children. Our review of existing literature on dietary and exercise interventions in women with obesity, either before or during pregnancy, revealed that these measures indeed offer a protective shield against the extent of this unhealthy heart development in children. Should these results hold into adulthood, these interventions could shield against the detrimental cardiovascular conditions seen in adult children of mothers with obesity, thus guiding public health strategies to enhance cardiovascular health for future generations.”
Although the data supports the premise that lifestyle adjustments in pregnant women with obesity may safeguard infant cardiovascular health, further comprehensive studies are necessary. These should involve larger cohorts and extend into later childhood to affirm the findings and assess if the benefits continue into adulthood.
Should future research corroborate these findings, the implications could be significant, potentially shaping public health initiatives aimed at improving heart health across generations.
Read More
Twenty years of research validates mediterranean diet’s role in lowering hypertension risk
A landmark study published in the European Journal of Clinical Nutrition has shed light on the enduring benefits of the Mediterranean diet in preventing hypertension (HTN) over an extensive 20-year period. Conducted among a group of initially non-hypertensive adults, this research marks a significant step in understanding long-term dietary impacts on health.
Hypertension remains a critical challenge globally, significantly influencing the onset of heart diseases and strokes, predominantly in low- and middle-income nations. Despite advancements in medication that stabilise blood pressure, approximately 30% of adults still suffer from HTN, which escalates both the healthcare costs and mortality associated with cardiovascular diseases (CVD). Lifestyle changes such as adopting balanced diets, regular physical activity, and smoking cessation are crucial for managing and preventing HTN. Official health guidelines recommend diets rich in plant-based foods, healthy fats, and lean proteins while being low in sodium and alcohol. The Mediterranean diet, celebrated since the 1960s for its role in preventing chronic conditions and reducing CVD mortality, has lacked long-term concrete evidence of its efficacy in managing blood pressure, prompting further investigation.
The study in question, known as the ATTICA study, complies with the Declaration of Helsinki and explores CVD incidence among Greek adults. Beginning in 2001-2002 with 4,056 individuals from the Attica region invited to participate, 3,042 agreed, embarking on a two-decade-long health journey. Initial assessments involved detailed face-to-face interviews at homes or workplaces by trained health professionals, who collected extensive socio-demographic, clinical, and biochemical data. Key health measures included fasting blood samples for glucose, insulin, total cholesterol, and high sensitivity C-reactive protein levels, among others. Participants also underwent physical examinations to ensure no pre-existing CVD and to measure blood pressure. Lifestyle factors including diet, exercise, and smoking habits were meticulously recorded, using a validated food frequency questionnaire to evaluate adherence to the Mediterranean diet through the MedDietScore.
Throughout the 20-year study period, participant engagement was maintained through regular follow-ups, with the latest in 2022 assessing 2,169 of the original cohort. This follow-up re-evaluated their health outcomes, including HTN, diabetes, and CVD development, corroborating data through family reports and medical records for deceased participants.
Statistical analyses utilised advanced software to contrast initial and 10-year dietary patterns, identifying four distinct adherence trajectories to the Mediterranean diet. Techniques such as correlation coefficients, chi-squared tests, and logistic regression models were employed to ascertain the connection between dietary adherence and HTN risk, accounting for variables like age, sex, body mass index, lifestyle habits, and initial health status.
Findings revealed that at the start, participants averaged 41 years of age with a near-equal gender distribution and showed moderate adherence to the Mediterranean diet, scoring an average MedDietScore of 27.1. Physically, 63.1% were minimally active, and about half were classified as having overweight or obesity. Early medical evaluations noted a 35.3% prevalence of hypercholesterolemia and a 3.9% incidence of diabetes.
Analysis of initial data highlighted a strong negative correlation between adherence to the Mediterranean diet and both systolic and diastolic blood pressures, indicating that higher dietary adherence correlated with lower blood pressure levels. Over the study’s duration, 314 individuals developed hypertension, representing a 22.2% incidence rate. Those who developed HTN typically were older, predominantly male, had higher obesity rates, poorer cardiometabolic profiles, and greater tobacco use compared to those who remained free from HTN.
In-depth analysis demonstrated that participants with low initial MedDietScore faced significantly higher HTN development rates than those with medium or high adherence levels. Statistical evaluation confirmed that each point increase in MedDietScore at baseline correlated with a 7% decrease in HTN risk over 20 years, a relationship that persisted even after adjusting for demographic and lifestyle factors.
The study also examined changes in diet adherence from the start to the 10-year point, revealing varied patterns. Notably, participants consistently adherent to the Mediterranean diet showed a remarkably lower incidence of HTN, with a 46.5% reduced risk in the fully adjusted model, underscoring the diet’s protective effect against HTN when sustained over time.
Read More
Adolescent stress linked to adult obesity and hypertension
Recent research indicates a strong correlation between high stress levels experienced during adolescence and the subsequent development of cardiometabolic risk factors, such as obesity and hypertension, in adulthood.
Published in the Journal of the American Heart Association, this study underscores the necessity of implementing stress management techniques from an early age. These strategies are vital in reducing the likelihood of health issues later in life, including heart disease and Type 2 diabetes.
Dr. Fangqi Guo, the lead author of the study and a postdoctoral research fellow at the University of Southern California’s Keck School of Medicine, emphasises the significance of understanding how stress perceived from childhood impacts the escalation of cardiometabolic risk factors in young adults. Dr. Guo’s findings reveal that long-term stress perception significantly influences various cardiometabolic aspects such as fat distribution, vascular health, and obesity. He stresses the importance of adopting stress management practices during adolescence to safeguard health.
Cardiometabolic risk factors, encompassing obesity, Type 2 diabetes or prediabetes, high cholesterol, and hypertension, often co-occur and are major contributors to cardiovascular disease. In 2020, cardiometabolic diseases, including cardiovascular conditions and Type 2 diabetes, were leading chronic health issues in the U.S., accounting for approximately 25% of all deaths, as per the American Heart Association.
The American Heart Association’s 2017 report highlighted that childhood adversities have long-term effects on cardiometabolic health. In recent decades, perceived stress has also been increasingly recognised as a contributing factor to cardiometabolic health problems.
In this new investigation, researchers analysed data from 276 individuals participating in the Southern California Children’s Health Study. The participants, initially enrolled by their parents between 2003 and 2014 at an average age of six, underwent health assessments during adolescence and as young adults from 2018 to 2021. Their average ages during these assessments were 13 and 24 years, respectively.
Each assessment included responses to a four-item Perceived Stress Scale, a widely utilised method for assessing stress-related feelings and thoughts over the previous month. For the youngest participants, stress levels were reported by their parents. The participants were then categorised into four groups based on their stress patterns: consistently high, decreasing, increasing, and consistently low.
The study’s evaluation of cardiometabolic health involved various health measurements, such as blood pressure and weight. Researchers also examined neck artery thickness to assess blood flow, haemoglobin A1C levels to determine diabetes status, and body fat percentage, with a focus on abdominal fat, a known risk factor for cardiovascular disease and Type 2 diabetes.
Participants who reported higher stress levels from their teenage years into adulthood were more prone to high blood pressure, increased total body fat, more abdominal fat, poorer vascular health, and a higher risk of obesity than those who experienced lower stress levels.
Dr. Guo expressed surprise at the consistency of the association between perceived stress patterns and various risk factors. He advocates for healthcare professionals to incorporate the Perceived Stress Scale in clinical assessments, allowing for early identification and treatment of individuals with elevated stress levels.
Read More
Pomegranate proves potent in metabolic health management
A comprehensive study featured in Nutrients journal has cast a spotlight on pomegranate (Punica granatum l., PG) and its polyphenolic compounds, scrutinising their potential to modulate metabolic irregularities. Historically embraced for its therapeutic properties against bacterial infections, diabetes, and various metabolic syndromes, pomegranate’s efficacy is being re-evaluated amidst concerns over the side effects of conventional pharmacological treatments.
The review delves into pomegranate’s pharmacokinetic profiles, safety, and bioavailability, particularly focusing on its capacity to combat metabolic disorders such as type 2 diabetes, obesity, dyslipidemia, and cardiovascular diseases. It outlines how PG’s consumption could attenuate insulin resistance, inflammatory cytokines, redox gene expression, blood pressure elevation, vascular damage, and lipoprotein oxidation.
In animal models, pomegranate seed oil has been found to reduce fat mass and enhance insulin sensitivity, corroborating previous research indicating significant reductions in lipid levels. The study further explains how enzymes and nuclear receptors involved in lipid metabolism are positively influenced by PG’s floral components.
Despite some contradictory findings regarding PG’s impact on food intake and weight gain, the review suggests genetic differences may account for varied physiological reactions to phytochemicals. PG polyphenols are also being explored for their anti-diabetic properties through diverse mechanisms, including modulation of PPAR-γ activity and adiponectin gene expression.
The review also evaluates the pharmacodynamics and safety of PG’s ellagitannin compounds, noting individual differences in urolithin production and absorption, which are influenced by factors such as gut microbiota composition and pH. Although high doses of PG have shown cellular and nuclear alterations in toxicological studies, conventional uses of PG and its compounds appear safe, with adverse effects only predicted at dosages exceeding those traditionally used in ethnomedicine.
In conclusion, the research indicates that PG could play a beneficial role in preventing metabolic disorders. However, the outcomes of clinical and pharmacokinetic studies remain variable, attributed to factors like plant part selection, cultivar differences, environmental conditions, bioavailability, organ accessibility, and individual genetic profiles. Despite these discrepancies, the therapeutic potential of PG in addressing components of metabolic syndrome highlights the need for integrated treatment strategies.
Read More
New study finds obesity in pregnancy raises risk of future heart disease
The link between maternal obesity and the long-term risk of cardiovascular disease has been further solidified by new research findings. A study led by Northwestern University in the United States has shone a light on the significant health risks faced by women who enter pregnancy with obesity.
The research team discovered that women with obesity before conception are more susceptible to complications during pregnancy than their counterparts with healthier pre-pregnancy weights. These complications include conditions like pre-eclampsia and gestational diabetes, which have previously been associated with an increased risk of heart disease later in life.
The study’s principal investigator, Dr. Sadiya Khan, emphasised that while these pregnancy-related issues can indeed signal future cardiovascular problems, they are not the underlying cause of heart disease. Instead, they merely highlight pre-existing risk factors that become apparent during the metabolic and physical demands of pregnancy.
To reach these conclusions, the researchers analysed health data from 4,216 women who were giving birth for the first time. They observed that those with higher body mass indices (BMIs) in the first trimester had an elevated risk of developing hypertensive disorders during pregnancy than those with BMIs within the normal range.
Dr. Khan explained that the study approached pregnancy as a ‘natural stress test’ for the heart, which could expose pre-existing health concerns. The implications of these findings underscore the importance of addressing pre-pregnancy obesity with proactive health interventions rather than waiting for cardiovascular events to occur.
The research team is advocating for healthcare providers to emphasise the importance of a nutritious diet and regular physical activity during prenatal visits. While weight loss is not recommended during pregnancy, guidance and support for maintaining an appropriate weight gain during this period are crucial.
The study also presented quantitative insights, revealing that among the participants, 4% had gestational diabetes and 15% encountered complications due to high blood pressure.
These findings, which align with prior research advocating for weight management during pregnancy through diet and exercise, have been published in the journal Circulation Research, providing valuable insights for expectant mothers and healthcare professionals alike.
Read More
Obesity-linked heart deaths triple in 20 years
Recent research disclosed a concerning surge in the number of US adults succumbing to heart disease where obesity was cited as a pivotal contributing factor, exhibiting a threefold rise between 1999 and 2020. This alarming revelation was documented in a study published in the Journal of the American Heart Association, leveraging data encapsulated in the comprehensive database curated by the Centers for Disease Control and Prevention (CDC).
Analysing death certificates facilitated a granular examination of the escalation in obesity-correlated cardiac deaths over the span of two decades. The researchers pinpointed a total of 281,135 heart disease fatalities attributed to obesity during the period under scrutiny. This translated to a tripling of the death rate, spiralling from a rate of 2.2 per 100,000 individuals to a significant 6.6 deaths per 100,000 populace, thereby showcasing a worrying trend in health outcomes related to obesity.
Ironically, this spike unfolded amidst a nearly 18 percent decrement in overall heart disease mortalities from 1999 to 2020, pointing towards a deep-seated issue relating specifically to obesity-linked cardiac ailments.
The racial and gender disparities were stark, with the black populace shouldering a higher mortality rate compared to other racial cohorts. Moreover, a gendered analysis revealed a preponderance of these deaths amongst males, albeit black females demonstrated a marginally elevated mortality rate relative to their male counterparts.
Obesity, delineated as a profound risk catalyst for heart disease, presently afflicts approximately 115 million individuals in the US, encompassing around 42% of the adult demographic and 20% of the juvenile population, as per CDC statistics. A decade-long observation underscores a rise by nearly 10% in adult obesity, illuminating the swelling magnitude of this health crisis.
Medical professionals accentuate the multifaceted pathways through which obesity can foster heart disease, encompassing the enhancement of blood pressure levels, fostering a surge in detrimental cholesterol whilst diminishing beneficial cholesterol levels, amplifying diabetes susceptibility, and facilitating the accrual of fatty substances within arterial structures.
The in-depth study unearthed that the primary culprits behind obesity-associated heart disease fatalities within the scrutinised period were ischemic heart disease — characterised by artery narrowing — accompanied by heightened blood pressure. This dual identification not only underscores the critical role of cardiovascular health monitoring in obesity management but also necessitates intensified focus on preventive measures to curb the steady increase in obesity-related cardiac deaths.
The findings evoke an urgent call for bolstered interventions targeting obesity prevention and management, steering individuals towards healthier lifestyles to avert the onset of associated cardiac complications. The study stands as a testament to the urgent necessity for a comprehensive approach in mitigating obesity-related health ramifications, fostering a society armed with the knowledge and resources to combat this escalating health concern effectively.
Read More
Digital health applications: A game-changer in post-hospitalisation heart failure care
According to a study published in the International Journal of Cardiology, the use of electronic health services via health applications after heart failure (HF) hospitalisation notably enhances patient outcomes and reduces mortality risk.
The research team aimed to scrutinise the effectiveness of digital health interventions (DHI) in comparison to conventional care for patients who had previously been hospitalised due to HF. To do this, they performed a retrospective study involving ten randomised controlled trials listed on databases such as MEDLINE, Cochrane, OVID, CINHAL, and ERIC. The trials studied the effects of DHI on patients with HF. The sample size comprised 7204 patients, predominantly men, with an average age of 65.7 years. These patients were followed for nearly 16 months, with all-cause death being the primary outcome measured.
Upon comparing the group utilising DHI with the standard care group, researchers discovered a reduction in all-cause mortality (8.5% vs. 10.2%; risk ratio [RR], 0.80; 95% CI, 0.66-0.96; P =.02) as well as cardiovascular mortality (7.3% vs. 9.6%; RR, 0.76; 95% CI, 0.62-0.94; P =.01). However, the study found no significant difference in HF-related hospitalisations (23.4% vs. 26.2%; RR, 0.82; 95% CI, 0.66-1.02; P =.07) and all-cause hospitalisations (48.3% vs. 49.9%; RR, 0.89; 95% CI, 0.77-1.03; P =.11).
Further, the DHI group experienced fewer lost days due to HF-related hospitalisations when compared with the standard care group (mean difference [MD], -1.77; 95% CI, -3.06 to -0.48; P =.01; I2 = 51). However, the number of days lost to all-cause hospitalisations was similar in both groups (MD, -0.76; 95% CI, -3.07 to -1.55; P =.52; I2 = 69).
The study had certain limitations, including reliance on study-level data rather than individual patient data, the meta-analysis research design, variability in certain study endpoints, and a lack of representation of women in the study group.
The authors of the study concluded, “This meta-analysis of randomised controlled trials supports a reduction in all-cause and cardiovascular mortality, with less total time spent in HF hospitalisations when DHI is employed in patients with prior HF hospitalisations.” They further highlighted the need for more extensive studies to examine different types of DHI and assess their cost-effectiveness in managing HF.
Read More
Common painkillers linked with heart failure in people with type 2 diabetes
A recent study published in the Journal of the American College of Cardiology suggests that the use of common pain medications such as Advil or Motrin (ibuprofen) may increase the risk of heart failure in people with type 2 diabetes. The study found that NSAIDs (nonsteroidal anti-inflammatory drugs) may lead to first-time hospitalisation for heart failure in patients with type 2 diabetes. This is noteworthy, as these individuals are already known to face an elevated risk of heart failure.
The Danish study included more than 330,000 individuals with type 2 diabetes, of whom 1 in 6 filled at least one NSAID prescription within a year. During a follow-up of almost six years, more than 23,000 subjects were hospitalised with heart failure for the first time, and NSAID use was associated with a 40 percent higher relative risk of first-time heart failure hospitalisation. Ibuprofen and diclofenac were found to increase the risk of heart failure hospitalisation, but not celecoxib and naproxen. There was no association of NSAID use and increased risk in people with well-controlled diabetes. Strong associations were found in people aged 65 and older, while no association was found in those younger than 65. The strongest association was found in very infrequent or new users of NSAIDs. The study highlights the need for education in patients with cardiac risk factors, such as diabetes, on the dangers of over-the-counter medications.
Read More