
Novo Nordisk’s weight-loss drug Wegovy demonstrates heart benefits in latest trial
Novo Nordisk’s groundbreaking obesity drug, Wegovy, has been shown to offer significant cardiovascular advantages, according to the results of a major late-stage trial announced on Tuesday (8th of August, 2023). This revelation not only highlights the efficacy of the medication but also helps in reshaping its perception beyond merely being a lifestyle drug.
The clinical study, named SELECT, revealed that individuals treated with Wegovy experienced a 20% reduction in the occurrence of heart attack, stroke, or death from heart-related diseases, in comparison to those who were administered a placebo. These findings far exceed the 15-17% reduction that had been anticipated by investors and analysts, although it’s worth noting that the results have not yet been subject to peer review.
Involving a substantial cohort of 17,500 participants, the SELECT trial specifically targeted individuals with overweight or obesity aged 45 or older, with a history of heart disease, but without prior diagnosis of diabetes. The trial, which spanned nearly five years, aimed to determine whether Wegovy’s weekly injection could confer tangible medical advantages.
The announcement of these positive results led to a surge in Novo Nordisk’s shares, propelling them by more than 13% to record highs. Over the past two years, the company’s shares have skyrocketed by almost 150%.
These encouraging outcomes could potentially influence insurers in the U.S. and health authorities in Europe to extend coverage of Wegovy to a broader segment of patients. Currently, some healthcare plans, including the U.S. Medicare health plan, categorise weight-loss treatments as lifestyle drugs. Experts opine that the new data might lead to a reassessment of this stance, particularly in the U.S., where the cost of Wegovy stands at $1,300 per month.
The findings from the trial have also prompted discussions regarding the long-term health benefits of the drug, particularly in terms of potentially lowering the overall healthcare burden and the expenses associated with treating heart disease in populations with overweight or obesity. Some experts, like Dr. Jeff Levin-Scherz, a consultant at Willis Towers Watson, remain cautious, suggesting that medical cost savings might be years away. He postulates that the drugs may prove to be cost-effective in improving patients’ lives but may not necessarily reduce their overall healthcare costs.
Large American corporations, which previously covered weight-loss treatments for their employees, have reduced their support due to escalating costs. However, the landmark data from the SELECT trial illustrates Wegovy’s potential to redefine how obesity is perceived and treated, according to Martin Holst Lange, Novo Nordisk’s executive vice president for development.
Novo Nordisk has expressed plans to submit applications for regulatory approvals of a label indication expansion for Wegovy in the U.S. and the European Union within the year.
Wegovy has already had a transformative impact on the weight-loss market since its U.S. introduction in June 2021. It has not only garnered attention from patients, investors, and celebrities around the globe but also significantly contributed to Novo’s shares’ growth. The injection helps patients feel fuller for more extended periods, resulting in an average weight loss of around 15% when coupled with dietary and exercise changes. The drug is part of the GLP-1 agonists class, initially developed to treat type 2 diabetes.
With obesity affecting over 650 million adults globally, a figure that has tripled since 1975, and approximately another 1.3 billion classified as having overweight, the World Health Organization links these conditions to heightened risks of heart disease and diabetes.
Industry analysts, like Sydbank’s Soren Lontoft Hansen, are optimistic that these better-than-expected results will cause a stir among physicians who prescribe anti-obesity drugs. Furthermore, Barclays analysts project that a positive outcome from the study could boost Wegovy’s uptake by 25% by 2030, provided it receives approval for expanded use.
Novo Nordisk is currently facing challenges to meet the soaring U.S. demand for Wegovy. In May, the company announced it was cutting the supply of starter doses to the U.S. market by half to secure supplies for existing patients. Although larger doses were reported to be in short supply by Reuters, Novo has denied such claims.
The detailed data from the trial is scheduled to be presented at a scientific conference later in 2023, and additional details may be revealed when Novo releases its second-quarter results on Thursday.
Read More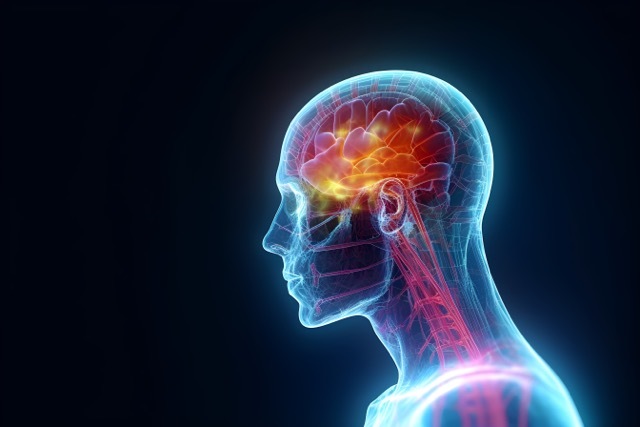
Hypothalamic differences discovered in people who are living with overweight or obesity
A groundbreaking study by researchers at the University of Cambridge has provided new insights into the role of the hypothalamus in controlling appetite. This small yet critical region of the brain, which is about the size of an almond, appears to have structural differences in those who are living with overweight or obesity compared to those of healthy weight.
Dr. Stephanie Brown from the Department of Psychiatry and Lucy Cavendish College, University of Cambridge, noted the importance of the hypothalamus in regulating appetite but also acknowledged the difficulty in studying it in living humans due to its small size.
The study team addressed this challenge by using a machine learning algorithm to analyse MRI scans of 1,351 young adults across different BMI categories. Published in Neuroimage: Clinical, their findings revealed that the hypothalamus’s overall volume was significantly larger in those who with overweight or obesity.
These findings offer further evidence to the connection between brain structure, weight, and food consumption, as obesity is a global concern affecting over 1.9 billion people worldwide. The condition increases risks for numerous health problems, including type 2 diabetes, heart disease, stroke, and mental health issues.
The team also explored the possibility that the changes in the hypothalamus might be related to inflammation. Previous animal studies have shown that a high-fat diet could cause inflammation in the hypothalamus, leading to insulin resistance and obesity. In some cases, just three days of a fat-rich diet was enough to trigger inflammation.
Dr. Brown emphasised that if similar processes occur in humans, a high-fat diet could impact our ability to sense when we’ve eaten enough, leading to weight gain. The researchers hypothesised that the brain might react to inflammation by enlarging specialised immune cells, known as glia, causing the hypothalamus to be larger.
Professor Paul Fletcher, the study’s senior author, expressed hope that this new approach to analysing brain scans would deepen our understanding of appetite control in obesity. While the exact implications of these findings are still unclear, more research is needed to confirm whether the increase in hypothalamic volume is a cause or result of being overweight, or if those with larger hypothalami are naturally inclined to eat more.
Supported by the Bernard Wolfe Health Neuroscience Fund, Wellcome, NIHR Cambridge Biomedical Research Centre, and additional funding from Alzheimer’s Research UK, the study presents a transformative view of obesity. It opens new avenues for exploring obesity from a neurological perspective, potentially revolutionising how obesity and overweight conditions are understood and treated. Future studies may provide essential insights into intervention strategies, reshaping the way we approach this global health challenge.
Read More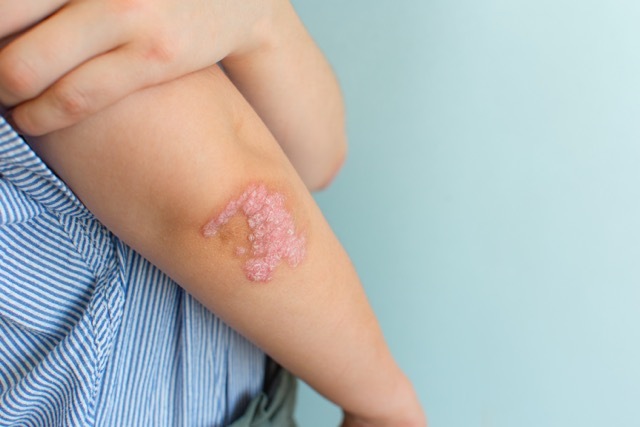
Obesity linked to impairment of immune cells protecting against psoriasis
Obesity is more than just a condition associated with excess weight; it can also influence the immune system in ways that make the body more susceptible to certain diseases. Recent research has shed light on how obesity may impair immune cells that protect against inflammation associated with psoriasis, a common skin disorder. This newfound understanding could pave the way for new treatments for psoriasis, particularly for those who suffer from obesity.
Psoriasis, marked by an accumulation of dry, scaly skin patches, is found to be twice as prevalent in individuals with obesity as compared to those without. This connection between obesity and psoriasis has long been observed, but the underlying mechanisms have remained elusive.
Researchers at Emory University in Atlanta, Georgia, led by Chaoran Li, took up the challenge to explore the intersection between obesity, inflammation, and psoriasis. They specifically investigated regulatory T-cells, which play a crucial role in controlling inflammation. These cells maintain a delicate balance in the skin, offsetting pro-inflammatory immune cells. While obesity is known to increase inflammatory cells, its influence on regulatory T-cells was not well understood.
Li’s team conducted a detailed genetic analysis of regulatory T-cells in various organs of mice, including the skin, spleen, lungs, and lymph nodes. They identified a unique subset of these cells that were prevalent in the skin of the rodents. Interestingly, this group was also found to be abundant in human skin samples.
The research took a significant turn when scientists genetically modified mice to lack these specific cells. When they applied a cream that induces psoriasis-like symptoms, such as skin thickening, the modified mice’s skin became nearly 50% thicker in a week compared to those with the anti-inflammatory cells. This observation strongly suggested that these particular cells have a role in preventing psoriasis symptoms.
To delve into the relationship with obesity, another group of mice were fed a high-fat diet for 16 weeks. The skin of these mice with obesity displayed fewer regulatory T-cells and was more reactive to the psoriasis-inducing cream than the skin samples from mice on regular diets. This correlation between obesity and a decrease in anti-inflammatory immune cells that prevent psoriasis was a pivotal discovery.
These findings not only highlight obesity’s impairment of crucial immune cells but also hint that a high-fat diet may be a key factor in psoriasis and other skin-related inflammations. This insight opens up the possibility that dietary interventions could be a viable treatment option for psoriasis.
Another promising avenue explored by the researchers involved the drug pioglitazone, known to boost the activity of regulatory T-cells. It was found to reduce skin inflammation in mice with obesity. Intriguingly, pioglitazone is also a type 2 diabetes medication. Some studies have indicated that individuals with diabetes on this drug have a lower risk of psoriasis, raising the potential of the medication as a dual-purpose treatment.
However, the applicability of these findings to humans still requires validation. Li’s team plans to examine how this specific subset of cells varies in humans with both psoriasis and obesity compared to those with one or neither condition.
This research represents a significant stride in understanding the intricate relationship between obesity, immune function, and psoriasis. By unearthing the cellular mechanisms behind this connection, it could potentially lead to more targeted and effective treatment options for those struggling with psoriasis, especially in the context of obesity. It also emphasises the importance of a healthy diet and its impact on overall skin health.
Read More
Revolutionising patient care: South Yorkshire’s cutting-edge digital health hub
Set to transform patient care, the South Yorkshire Digital Health Hub is a groundbreaking £4 million project with ambitious goals. It aims to revolutionise the treatment and diagnosis of diseases for a population of 1.4 million people living in a region heavily impacted by high disease prevalence and pronounced health inequalities. This initiative, led by the University of Sheffield, leverages innovative digital technologies to shape the future of healthcare.
Utilising state-of-the-art tools and techniques, the hub intends to pioneer cutting-edge research using data gleaned from smartphones, wearables, novel sensors, and the National Health Service (NHS) data. In addition to these, artificial intelligence (AI) will play a crucial role in the development of new clinical tools. This paradigm shift is set to redefine personalised patient care and facilitate disease management effectively.
The South Yorkshire Digital Health Hub has an impressive roster of partners, including Sheffield Hallam University, Sheffield Teaching Hospitals, local General Practitioners (GPs), mental health services, the Sheffield Integrated Care System, businesses, and patient and public groups. The collective intelligence of these stakeholders will forge a robust knowledge pool, capitalising on the region’s existing prowess in developing digital health technologies.
The Hub, among five across the UK, has been granted part of £16.5 million from the Engineering and Physical Sciences Research Council (EPSRC) and the Health Ageing and Wellbeing and Tackling Infections UKRI Strategic Themes. This financial backing aims to address four central healthcare challenges: antimicrobial resistance, disease prediction, diagnosis and intervention, out-of-hospital care, and tackling health disparities through the development and deployment of digital healthcare technologies.
The project targets both urban and rural populations, working towards addressing the unique healthcare needs shaped by significant health and social inequalities. Simultaneously, it offers a blueprint for stimulating economic growth in the region through digital skills training, networking, and knowledge exchange, bridging various stakeholders in the digital health sphere.
The South Yorkshire Digital Health Hub also proposes to deliver specialist health training online, accessible freely to researchers, clinicians, patients, and the public. Professor Tim Chico, Director of the South Yorkshire Digital Health Hub and Professor of Cardiovascular Medicine at the University of Sheffield, underscored the urgency of this investment. He emphasised the critical role of this state-of-the-art health technology research in tackling health disparities and high disease burden, including heart and lung diseases, cancer, and mental health issues prevalent in the region.
Echoing his sentiments, Professor Steve Haake, Deputy Director of the Digital Health Hub, envisions a future where digital health tools leverage real-time data from daily life. This transformation empowers patients and healthcare professionals to make informed decisions in a timely manner. Under the aegis of the hub, patients, clinicians, companies, and the public will have the autonomy to design their own apps and tools, bolstering their successful integration within the NHS.
Local authorities have thrown their weight behind the establishment of the South Yorkshire Digital Health Hub. Oliver Coppard, Mayor of the South Yorkshire Combined Authority, hailed the initiative as an instrumental step towards confronting health inequalities plaguing the region. He lauded the collaborative efforts between the NHS, universities, and the business community in highlighting South Yorkshire’s cutting-edge health and wellbeing sector, asserting its role as a global frontrunner in healthcare innovation.
Forming part of a more extensive £36.5 million investment in healthcare technology from the EPSRC, the Digital Healthcare Hubs, including the South Yorkshire Digital Health Hub, aim to spearhead innovative healthcare solutions. By leveraging advancements in robotics, computer modelling, and imaging, these hubs are set to redefine healthcare outcomes.
The South Yorkshire Digital Health Hub, with its robust collaboration among diverse stakeholders and focus on digital technologies, stands at the forefront of healthcare innovation. By addressing gaps in healthcare delivery and harnessing digital innovation, the hub holds significant promise in reshaping patient care, not only in South Yorkshire but far beyond its borders.
Read More
Pioneering digital health startups target U.S. maternal health challenges
The escalating maternal health crisis in the U.S., highlighted by a disconcerting 40% surge in maternal deaths during or shortly after pregnancy to 1,205 in 2021, is instigating an urgent response from the digital health sector. Startups like Pomelo Care, Maven Clinic, and Babyscripts are harnessing virtual services to bridge the maternal care gaps and mitigate pregnancy-related complications, according to the National Center for Health Statistics.
This alarmingly high mortality rate was a significant topic at The Wall Street Journal Health Forum in March. Here, Chelsea Clinton, through her venture-capital firm Metrodora Ventures, stressed the imperative need for intensified support towards women’s health. Clinton is an investor in Oula Health, a startup that’s diving into the sphere of maternal care.
Reports from the Centers for Disease Control and Prevention suggest that 80% of pregnancy-related deaths in the U.S. could have been prevented. Major underlying causes of these fatalities include mental health disorders, heart conditions, and hypertensive disorders during pregnancy.
Digital health startups aim to leverage telehealth and app technologies to identify and manage these health conditions proactively, thereby preventing potentially fatal complications. While technology isn’t the panacea, it undeniably enhances access to medical services and compensates for the scarcity of healthcare professionals, thereby promoting equitable care delivery.
Dr. Kathaleen Barker, an Assistant Professor of Obstetrics and Gynecology at UMass Chan Medical School-Baystate, emphasised the role of technology in equalising access to prenatal care. Baystate Health, a healthcare system in Western Massachusetts, utilises Babyscripts technology.
Investor-backed Babyscripts, headquartered in Washington D.C., collaborates with over 70 U.S. health systems. Co-founder and Chief Executive Anish Sebastian stated that Babyscripts, also known as 1EQ, offers patients a blood-pressure monitor that pairs with an app via Bluetooth. This technological intervention aims to preempt conditions such as preeclampsia, a condition characterised by high blood pressure and signs of liver or kidney damage that can arise after the 20th week of pregnancy.
Pomelo Care, a New York-based virtual clinic, aims to supplement in-person care by providing services between doctors’ appointments. Having secured $33 million in seed and Series A funding led by Andreessen Horowitz, Pomelo Care assigns a nurse to each patient to oversee their care. After assessing the patient’s needs and health claims data, the nurse assembles a personalised care team.
Pomelo Care operates on a value-based business model that encourages improving patient access to care, enhancing outcomes, and reducing costs. The company plans to validate its effectiveness through studies conducted in collaboration with insurers and academic medical centres, with the findings set to be published.
Another player in the field, Maven Clinic, grants virtual access to an array of services, such as doulas, midwives, physical therapists, and mental health care. Maven has devised a tool to screen for social needs like access to housing, food, and essentials for the family and baby.
The stark truth is that women’s health has been neglected in the U.S., resulting in many women living in maternal-care deserts where access to services is challenging. The conversation about this issue is just starting at the national level, noted Kate Ryder, founder, and CEO of Maven Clinic. However, these innovative digital health startups are undoubtedly setting the stage for a more promising, tech-driven future in maternal healthcare.
Read More
Revolutionary AI tool forecasts pancreatic cancer risk up to three years in advance
Ground-breaking research spearheaded by Harvard Medical School, in collaboration with the University of Copenhagen, VA Boston Healthcare System, Dana-Farber Cancer Institute, and the Harvard T.H. Chan School of Public Health, has developed an artificial intelligence (AI) instrument capable of identifying individuals at the greatest risk of developing pancreatic cancer up to three years before diagnosis, using solely their medical records.
The study, published in Nature Medicine on May 8, indicates that implementing AI-driven population screening could be a key strategy in detecting those at a high risk of pancreatic cancer earlier. This could, in turn, hasten the diagnosis of a condition often detected at advanced stages when treatment options are less effective, resulting in poorer outcomes. Pancreatic cancer, one of the world’s deadliest malignancies, is anticipated to increase its mortality toll.
At present, there is an absence of population-wide screening tools for pancreatic cancer. Targeted screenings are performed for individuals with certain genetic mutations or a family history that increases their risk of developing the disease. However, these screenings may overlook other cases not fitting these criteria, the researchers highlighted.
The study’s co-senior investigator, Chris Sander, a faculty member in the Department of Systems Biology at the Blavatnik Institute at HMS, underscored the significance of the AI tool. “Deciding who is at a high risk for a disease and would benefit from additional testing is one of the most challenging determinations clinicians have to make. The tests can be more invasive, more costly, and carry their own risks. An AI tool that accurately identifies those at the highest risk for pancreatic cancer and who would gain the most from additional tests could greatly enhance clinical decision-making.”
If implemented widely, this AI-driven method could expedite the detection of pancreatic cancer, lead to earlier treatment, and improve patient outcomes, possibly extending their life spans.
“AI-driven screening provides the opportunity to change the course of pancreatic cancer, a formidable disease that is exceptionally challenging to diagnose early and treat promptly,” said study co-senior investigator Søren Brunak, a professor of disease systems biology and research director at the Novo Nordisk Foundation Center for Protein Research at the University of Copenhagen.
In this novel study, the researchers trained the AI algorithm on two separate data sets, containing a total of 9 million patient records from Denmark and the United States. They instructed the AI model to identify potential signs of pancreatic cancer risk based on the data in the records.
The model could predict patients likely to develop pancreatic cancer in the future by identifying combinations of disease codes and the timing of their occurrence. Interestingly, many of the symptoms and disease codes were not directly related to or derived from the pancreas.
The researchers evaluated different versions of the AI models for their capacity to identify individuals at a heightened risk of disease development over different timescales – 6 months, one year, two years, and three years.
Overall, each iteration of the AI algorithm proved considerably more precise in predicting who would develop pancreatic cancer than current estimates of disease incidence in the general population. The researchers proposed that the model is likely as accurate in predicting disease onset as the existing genetic sequencing tests, which are generally only accessible to a small subset of patients in data sets.
Screening techniques for certain prevalent cancers, such as breast, cervix, and prostate cancer, rely on relatively straightforward and highly effective techniques, such as a mammogram, a Pap smear, and a blood test. These methods have significantly improved the outcomes for these diseases by ensuring early detection and intervention.
In contrast, pancreatic cancer poses greater challenges and costs in terms of screening and testing. Doctors predominantly focus on family history and the presence of genetic mutations. While these are crucial indicators of future risk, they often overlook many patients.
The AI tool presents a significant advantage in its potential applicability to any patient for whom health records and medical history are available, not solely those with a known family history or genetic predisposition for the disease. This is particularly important, the researchers noted, because many patients at a high risk may not be aware of their genetic predisposition or family history.
In the absence of clear indications that a person is at high risk for pancreatic cancer and without symptoms, clinicians may understandably hesitate to recommend more sophisticated and costlier testing methods such as CT scans, MRI, or endoscopic ultrasound.
When these tests are performed and suspicious lesions are detected, the patient must undergo a procedure to obtain a biopsy. Given its deep placement in the abdomen, the pancreas is difficult to reach and easy to inflame, leading to its nickname as “the angry organ.”
The researchers advocate for an AI tool that singles out those at the greatest risk for pancreatic cancer. This would ensure clinicians are testing the correct population, while also preventing others from undergoing unnecessary testing and additional procedures.
The survival rate for those diagnosed with pancreatic cancer in its early stages is about 44 percent, five years post-diagnosis. However, only 12 percent of cases are diagnosed at this stage. The survival rate decreases dramatically to 2 to 9 percent for those with tumours that have spread beyond their origin, the researchers estimated.
Chris Sander emphasised, “Despite significant advancements in surgical techniques, chemotherapy, and immunotherapy, the survival rate remains low. Therefore, besides advanced treatments, there’s a pressing need for better screening, more focused testing, and earlier diagnosis. This is where the AI-based approach serves as the initial critical step in this process.”
For the current study, the researchers created multiple versions of the AI model and trained them on the health records of 6.2 million patients from Denmark’s national health system over a 41-year span. Of these patients, 23,985 developed pancreatic cancer over time.
During the training, the algorithm identified patterns suggesting future pancreatic cancer risk based on disease trajectories. For instance, diagnoses such as gallstones, anaemia, type 2 diabetes, and other gastrointestinal-related issues pointed to a higher risk for pancreatic cancer within three years of evaluation.
Inflammation of the pancreas was a strong predictor of future pancreatic cancer within an even shorter time span of two years.
The researchers caution that none of these diagnoses on their own should be deemed indicative or causative of future pancreatic cancer. However, the pattern and sequence in which they occur over time provide clues for an AI-based surveillance model and could prompt physicians to closely monitor or test those at elevated risk.
Next, the researchers tested the best-performing algorithm on an entirely new set of patient records it had not previously seen — a U.S. Veterans Health Administration data set comprising nearly 3 million records over 21 years, including 3,864 individuals diagnosed with pancreatic cancer.
The tool’s predictive accuracy was somewhat lower on the US data set. The researchers attributed this to the shorter collection period and the different patient population profiles in the U.S. dataset compared to the Danish dataset.
When the algorithm was retrained from scratch on the U.S. dataset, its predictive accuracy improved. This, the researchers said, underscores the importance of training AI models on high quality, rich data and the necessity of access to large representative datasets of clinical records aggregated nationally and internationally.
In the absence of globally valid models, AI models should be trained on local health data to ensure their training reflects the specific characteristics of local populations.
Read More
New report illuminates the promising role of cloud technology in healthcare
A fresh report spotlighting the transformative role of cloud technology in combating the prevalent challenges in healthcare has been released by the Health Policy Partnership. The publication, titled “Our Health in the Cloud: Exploring the Evolving Role of Cloud Technology in Healthcare,” outlines the practical application of this technology. The report was created with the support of the European Institute for Innovation through Health Data (i~HD).
The publication coincides with the HIMSS 2023 European Health Conference & Exhibition in Lisbon, and delves into how cloud technology has propelled innovative solutions within the healthcare industry, and its potential future contributions.
Dipak Kalra, president of the i~HD, commented, “Cloud technology is a crucial catalyst for leveraging health data to enhance health outcomes, boost patient safety, swiftly identify public health threats, and expedite research into novel medicines and medical technologies.”
“Cloud technology offers secure computational power surpassing conventional on-premise resources, facilitating data integration across entities. Our report seeks to express why health decision-makers should be concerned about cloud technology, what they need to comprehend and be assured about urgently, and how to progress in a manner that prioritises the needs and preferences of patients and the public in health sector’s cloud integration,” Kalra added.
Cloud technology plays a pivotal role in enabling the data-centric strategy currently prevalent in healthcare. It has already demonstrated its potential in the field, offering key advantages like improved efficiency in patient-focused care, a population-oriented health approach, research that sparks innovation, and durable, resilient health systems.
However, the report highlights the industry’s lack of general awareness and comprehension of cloud technology. This lack of understanding leads to perceived risks, such as those related to privacy and security, which continue to hinder its broad adoption.
Suzanne Wait, Managing Director at The Health Policy Partnership, stated, “As both healthcare delivery and research have become increasingly data-intensive and collaborative, the process of gathering, merging, storing, analysing, and exchanging these data demands computational power, cybersecurity, and speed that far surpass typical onsite capacities, thus necessitating cloud technology. All stakeholders, not just IT departments, should enhance their understanding of ‘the cloud’ and ensure its proper and maximal usage across healthcare settings.”
The report emphasises the necessity for both patients and healthcare professionals to actively participate in discussions and policymaking concerning the technology. This involvement is key to ensuring that its implementation caters to their needs and incorporates their perspectives.
According to a recent report from Netskope Threat Labs, the healthcare sector has a comparatively low count of cloud malware downloads relative to other sectors. However, as cloud technology’s deployment expands, it is crucial for organisations to ensure they are adequately protected.
Read More
Innovative ear-mounted cameras: Revolutionising dietary monitoring and advice
A group of scientists are working on an unprecedented approach to dietary tracking, drawing inspiration from the concept of constant surveillance. The researchers are creating minute cameras that can be attached to the ear, recording every food item consumed by the wearer.
The camera’s footage will be processed by an artificial intelligence (AI) system that can identify both the type of food and portion sizes. The ultimate objective is to provide customised advice on dietary habits, bridging the gap in dietary research that has often relied on participants’ unreliable self-reporting via surveys or diaries. The common issues include forgetfulness in recording meals, inaccuracies in estimating portion sizes, and intentional omissions due to feelings of guilt, particularly with regard to treats and alcohol.
The Health Survey of England 2021 stated that approximately 25.9% of adults had obesity, with an additional 37.9% classified as having overweight. Obesity is linked to a variety of health issues, including depression, infertility, hypertension, cancer, dementia, heart failure, and type 2 diabetes. The latter condition significantly raises the risk of blindness, peripheral neuropathy, and limb amputation.
Predictions for 2035 suggest that the NHS will likely spend more on treating diet-related type 2 diabetes than on all types of cancer. However, despite nearly 700 policy interventions implemented between 1996 and 2020 to curb national weight gain, as cited by former government food tsar Henry Dimbleby, obesity rates continue to rise.
According to Professor Gary Frost, the Head of Nutrition Research at Imperial College London, “There is a glaring gap in our understanding of people’s daily dietary habits. The current tools for dietary tracking are inaccurate, making it challenging to discern the connection between diet and disease.”
The innovative project, named CoDiet, also plans to evaluate urine and blood samples to study the correlations between dietary habits, bodily changes, and the onset of diseases such as type 2 diabetes. A primary goal is to develop a tool using AI that can dispense diet advice specific to an individual’s needs.
“We anticipate the ability to formulate new individual-focused policies to counteract common diseases related to lifestyle,” Frost said.
Scheduled to commence in September (of 2023), the project will initially use the ear-mounted cameras to record the dietary practices of 50 British volunteers and an additional 150 participants from Cork in the Republic of Ireland, Spain, and Greece.
Read More
Rising obesity prevalence may have altered perceptions of healthy body weights, study suggests
A concerning trend has emerged, revealing that an increasing number of overweight teenagers do not perceive themselves as being too heavy. This phenomenon raises alarms as it may lead to detrimental lifestyle choices, warn scientists. The trend of underestimating body weight was found to be particularly prevalent among girls, according to a peer-reviewed study.
The study suggests that the rising prevalence of obesity and the emergence of body trends idealising an athletic, muscular physique may contribute to teenagers underestimating their weight and becoming resistant to adopting healthy diet and exercise habits. However, the researchers acknowledge that other factors, including body image, dieting, changing eating patterns, and migration, may also play a role in these shifting perceptions over time.
Conducted by the International Health Behaviour in School-Aged Children, the study surveyed 11 to 15-year-olds between 2002 and 2018, analysing trends in body weight perception while considering age, gender, and family socioeconomic status. The survey encompassed over 745,000 adolescents from 41 countries across Europe and the United States. These findings are particularly significant for the UK, where more than a third of teenagers have either overweight or obesity.
Lead author of the study, Dr. Anouk Geraets from the Department of Social Sciences at the University of Luxembourg, emphasised the potential impact of body weight perception during this impressionable age on teenagers’ lifestyle choices, including their food consumption and exercise habits. Dr. Geraets expressed concern regarding the trend of fewer adolescents perceiving themselves as overweight, as this could undermine efforts to address the escalating obesity levels among this age group. Teenagers who underestimate their weight may not recognize the need to lose excess weight and may consequently make unhealthy lifestyle choices.
The study revealed an increase in underestimation of weight status and a decrease in overestimation over time, with girls being more susceptible to these perceptions than boys. Scientists worry that shifting trends in perception could diminish the effectiveness of public health interventions targeting young people.
Dr. Geraets emphasised the clinical and public health implications of the study. While the increase in accurate weight perception and the decrease in overestimation may have a positive impact by reducing unnecessary and unhealthy weight loss behaviours among adolescents, the rise in underestimation highlights the need for interventions to strengthen accurate weight perception. Further research is necessary to understand the underlying factors driving these trends and to develop effective public health interventions.
The study’s findings were published in the journal Child and Adolescent Obesity, shedding light on the urgent need to address teenagers’ misperceptions of their weight in order to promote healthier lifestyles and combat the growing obesity crisis among this age group.

Study challenges belief that moderate alcohol consumption shields against obesity and type 2 diabetes
Moderate alcohol consumption does not provide protection against conditions such as obesity and type 2 diabetes, according to a recent study, challenging the long-debated notion of potential health benefits associated with light to moderate drinking.
The study investigated whether modest alcohol intake had any positive effects on health—a subject that has divided experts. Researchers analysed data on alcohol consumption from over 400,000 participants and discovered a higher risk of obesity and type 2 diabetes among individuals who consumed more than 14 drinks per week. Notably, this link was more pronounced in women than in men.
Dr. Tianyuan Lu of McGill University in Québec commented on the findings, stating, “Previous research has suggested that moderate drinkers may be less susceptible to developing obesity or diabetes compared to non-drinkers and heavy drinkers. However, our study indicates that even light-to-moderate alcohol consumption, defined as no more than one standard drink per day, does not safeguard against obesity and type 2 diabetes in the general population.”
The study’s results revealed that heavy drinking was associated with increased measures of obesity, such as body mass index, waist-to-hip ratio, and fat mass, as well as an elevated risk of type 2 diabetes.
Importantly, the study did not find any evidence of improved health outcomes related to moderate alcohol consumption in individuals who consumed seven or fewer alcoholic drinks per week.
Dr. Lu concluded by highlighting the significance of the research in promoting awareness of the risks associated with alcohol consumption. The study’s findings aim to inform future guidelines and recommendations regarding alcohol use, with the hope of encouraging healthier behaviours as alternatives to drinking.
For further details, refer to the full study published in JCEM.
Read More
Scientists call for government action on portion sizes to tackle childhood obesity
Leading scientists are urging the government to establish standard portion sizes for young children as part of efforts to combat the obesity epidemic. In a damning report, government scientific advisers have revealed that young children are consuming excessive amounts of salt and sugar while falling short on fruit, fibre, and vegetable intake.
Official data indicates that one in ten reception-age children in the UK now has obesity, with experts projecting that the obesity crisis will cost the NHS £10 billion annually by 2050. The report from the Scientific Advisory Committee on Nutrition (SACN) highlights the absence of formal guidance on appropriate portion sizes for young children and emphasises the need for policymakers to address this issue. Oversized servings are contributing to the rapid consumption of excessive calories.
According to the report’s authors, the current diet of young children in the UK fails to meet the recommended dietary guidelines for several nutrients. They note that larger portion sizes of snacks and meals provided in preschool settings are associated with higher food and energy intake in the short term. To address these concerns, the authors recommend that the government consider developing age-appropriate portion sizes for food and beverages, including vegetables, fruit, fruit juice, and milk, targeting children aged 1 to 5 years.
The SACN, known for its advocacy of the forthcoming ban on fast-food advertising before 9 pm from 2025 and the fortification of bread with folic acid, has identified excessive sugar consumption as a widespread issue, leading to dental problems that pose long-term health risks for individuals and place a persistent burden on the NHS.
The report reveals that nutritional imbalances are prevalent in the average diet, with children from disadvantaged backgrounds experiencing even worse dietary quality. Commissioned by the Department for Health and Social Care, the report provides the first update on recommended food and beverage consumption for children aged one to five in nearly two decades. Based on a comprehensive review of two decades of studies and data, the panel of nutrition experts and paediatricians who form the SACN made several recommendations, highlighting the urgency of addressing the “high prevalence” of overweight and obesity in children in the UK.
Official figures indicate that approximately 3% of reception-age children have severe obesity, and one in ten children at this age meet the threshold for obesity.
The report authors also suggest that repeated exposure to initially disliked vegetables can help children develop a preference for them. They recommend that parents persistently offer the vegetable to their child eight to ten times to increase acceptance.
Additional recommendations from the report include avoiding fizzy drinks for children under the age of five, consuming unsweetened yoghurt products, and making milk and water the primary beverage choices. Semi-skimmed cow’s milk is acceptable, but fully skimmed milk should be avoided until age 5.
Bridget Benelam, a Nutrition Scientist from the British Nutrition Foundation, highlighted the report’s findings, stating that the diets of 1-5-year-olds were inadequate, characterised by excessive sugar, salt, and unhealthy energy-dense foods, and insufficient fibre, fruit, and vegetables.
The report also emphasises the importance of early childhood nutrition, not only for growth and development but also for establishing healthy habits that will benefit children later in life.
The report suggests several strategies for the government to consider, including promoting continued breastfeeding into the second year of life, ensuring children receive daily vitamin D and A supplements, and providing adequate vitamins and minerals for vegan families who may lack these nutrients commonly found in animal products.
A government spokesperson acknowledged that the report’s recommendations are being noted and considered. They highlighted the Start for Life resources, which provide expert NHS advice, helpful videos, and simple recipe ideas to support families in providing healthy meals for babies and young children.
Read More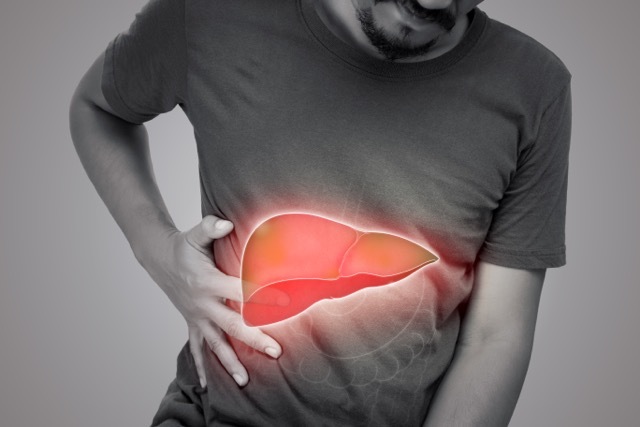
UK’s soaring liver cancer death rate blamed on alcohol and obesity
Liver cancer deaths in the UK have seen a staggering 40% increase over the past decade, making it the fastest-growing cause of cancer-related fatalities in the country, warns the British Liver Trust. Calling attention to the alarming rise, the charity is urging immediate measures to address the “carcinogenic effects” of inexpensive alcohol and unhealthy food.
Pamela Healy, CEO of the British Liver Trust, identifies alcohol and obesity as the key drivers behind the surge in liver cancer cases and deaths. She stresses the need for government intervention to combat these issues, asserting that such action can create a healthier environment for all. Healy emphasises the urgency of addressing the accessibility and affordability of unhealthy food, often priced significantly lower than nutritious alternatives.
This call for action comes amidst delays in implementing regulations that would prohibit supermarket multi-buy deals on high-fat, high-sugar, or high-salt foods. The Association of Directors of Public Health has also urged ministers to introduce minimum unit pricing on alcohol, following Scotland’s successful implementation of a minimum price of 50p per unit in 2018.
The British Liver Trust has submitted evidence to the parliamentary health and social care committee’s inquiry into future cancer care, focusing on innovative approaches to diagnosis and treatment. In addition to advocating for earlier detection and improved access to effective therapies, the charity emphasises the importance of prevention. Liver disease, a significant risk factor for liver cancer, can be reversed through lifestyle modifications, including reduced alcohol consumption and weight loss.
The submission by the British Liver Trust emphasises the need for upstream interventions to mitigate the carcinogenic impact of an unhealthy food and beverage environment. The charity cites evidence indicating that population-wide measures regulating the affordability and accessibility of alcohol and unhealthy food are more effective in reducing disease burden and addressing health inequalities than individual behaviour change alone.
The charity calls for a comprehensive alcohol strategy that tackles promotions and affordability. It highlights the fact that alcohol is classified as a group 1 carcinogen, known to cause at least seven types of cancer. Data from Cancer Research reveals that liver cancer mortality rates per 100,000 people in the UK have risen from 6.4 in 2007-2009 to 9.3 in 2017-2019. Primary liver cancer has one of the lowest survival rates among all cancers.
The British Liver Trust emphasises the need for enhanced surveillance of high-risk groups with liver disease to enable early diagnosis and improve survival rates. Additionally, the charity advocates for increased investment in liver cancer research.
The UK government is facing mounting pressure to take more effective action to combat obesity. Danone UK and Ireland, one of the country’s major food companies, recently suggested that the government should consider taxing products high in fat, sugar, or salt to tackle the obesity crisis.
In response to the inquiry, the Department of Health and Social Care affirms its commitment to diagnosing 75% of cancers at stages 1 and 2 by 2028. The department outlines its interventions, including community health liver checks for those at high risk of cirrhosis, with a particular focus on deprived communities.
A spokesperson from the Department of Health and Social Care highlights ongoing efforts to encourage healthier food and drink choices and tackle obesity. Recognising that obesity costs the NHS approximately £6.5 billion per year and is the second leading cause of cancer, the spokesperson highlights initiatives such as calorie labelling in restaurants, cafes, and takeaways to empower individuals to make informed lifestyle choices.
The spokesperson further notes that the NHS has witnessed record numbers of cancer patients in recent years, with earlier-stage diagnoses becoming more prevalent. To support this, the government is strengthening the cancer workforce and has published the first-ever Long-Term Workforce Plan, backed by over £2.4 billion, aiming to deliver the most extensive training expansion in NHS history over the next 15 years.
Read More